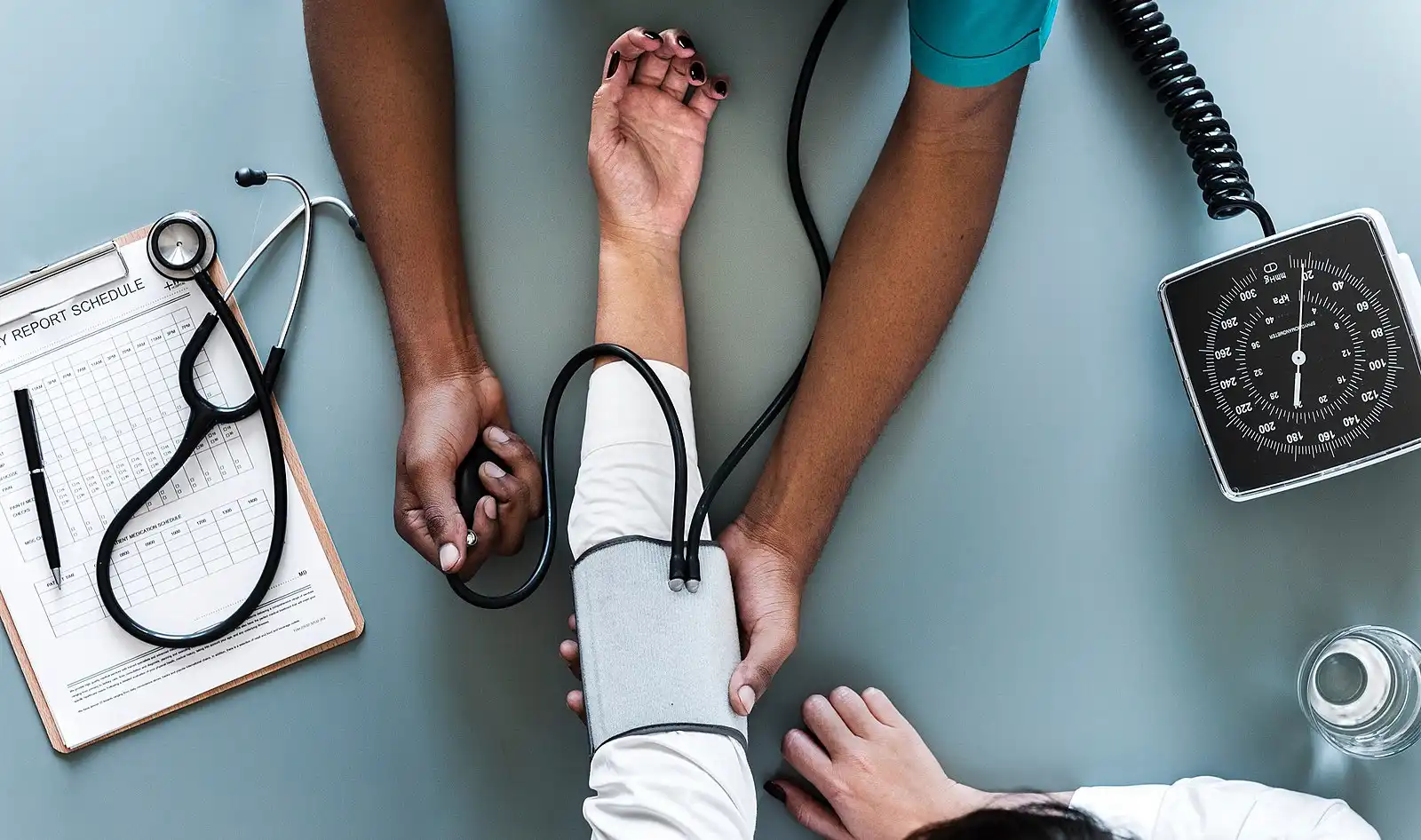
The vital signs include blood pressure, heart rate (pulse) and rhythm, respiratory rate and temperature. Baseline vital signs should be obtained before the start of dental treatment.
Blood pressure, heart rate and rhythm and respiratory rate provide information about the status of the cardiovascular system and should be recorded as an integral part of the routine physical evaluation. Recording of temperature is desirable but is currently considered optional and is done in situations deemed necessary, such as, when the patient appears febrile or infection is present.
Blood pressure
Blood pressure is based on the Korotkoff sounds produced by the passage of blood through obstructed, partially obstructed, or unobstructed arteries.
- Positioning of the patient : Patients should be seated in an upright position. Their arm should rest at the level of the heart, relaxed, slightly flexed, and supported on a firm surface. The patient should be permitted to rest for at least 5 minutes before the blood pressure is recorded. This allows the patient to relax so that the blood pressure recorded is closer to the patient's usual baseline reading.
- Placement of BP cuff : It should be deflated before it is placed on the arm. The cuff should be wrapped evenly and firmly around the arm, with the center of the inflatable portion over the brachial artery and the rubber tubing along the medial aspect of the arm. The lower margin of the cuff should be placed approximately 1 inch (2.5 cm) above the antecubital fossa.
- A cuff is too tight if two fingers cannot fit under the lower edge of the cuff. A tight cuff decreases venous return from the arm, which results in erroneous measurements (elevated diastolic pressure). A cuff is too loose if it can be pulled off the arm with only a gentle tug.
Palpatory systolic pressure
- The radial pulse is palpated in the wrist while the pressure in the cuff is increased rapidly to a point approximately 30 mm Hg above the point at which the radial pulse disappears.
- The cuff is then deflated slowly at 2-3 mm Hg per second until the radial pulse reappears. This gives the palpatory systolic pressure.
Auscultatory method
- The diaphragm of the stethoscope is placed firmly on the medial aspect of the antecubital fossa over the brachial artery. To reduce noise, the stethoscope should not touch the BP cuff or rubber tubing.
- The BP cuff should be inflated rapidly to a level of 30 mm Hg above the previously determined palpatory systolic pressure.
- Pressure in the cuff should be released gradually (2-3 mm Hg per second) until the first sound is heard through the stethoscope. A light tapping sound is heard as the pressure decreases. This pressure at which this first sound occurs is the systolic BP.
- As the cuff deflated further, the sound changes in quality and intensity. The sounds become dull and muffled and then cease as the pressure approaches diastolic BP. The diastolic BP can be determined best as the point at which the sounds cease completely. However, in some instances the sounds do not disappear completely. In such cases, the point at which sounds become muffled serves as the diastolic pressure.
- The cuff should be deflated slowly to a point 10 mm Hg beyond the point of disappearance and then totally deflated.
- If additional recordings are necessary, at least 15 seconds should elapse before the cuff is reinflated. This allows the blood trapped in the arm to flow elsewhere, providing a more accurate subsequent reading.
Common Errors
- Loose application of the BP cuff : Most common error, results in false elevated reading.
- Use of wrong cuff size : An adult BP cuff placed on an obese patient's arm produces falsely elevated readings, while the same cuff applied to the arm of a child or thin adult produces falsely decreased readings. The width of the cuff should be approximately 20% greater than the diameter of the extremity on which it is being used.
- Auscultatory gap : Represents a loss of sound between systolic and diastolic pressures, with the sound reappearing at a lower level. It can be avoided through the use of the palpatory method prior to the auscultatory method, as pulse is palpable in the gap even when the sound disappears. Although the auscultatory gap has no pathologic significance, it is found most often in patients with high BP.
- Measurement in anxious patient : Anxiety may cause transient elevations in blood pressure, primarily systolic pressure secondary to endogenous catecholamine release.
- Watching the needle on an aneroid manometer for pulsations : Leads to recording of falsely elevated systolic pressures, as these pulsations are commonly noted approximately 10-15 mmHg before the initial Korotkoff sounds are heard.
- Use of the right or left arm produces differences in recorded BP. A difference of 5-10 mmHg exists between the arms, with the left arm commonly producing slightly higher measurements.
Guidelines for clinical evaluations
Adult patients with the BP in the ASA 1 range, should have their BP rechecked every 6 months. For ASA 2, the BP should be rechecked before dental treatment for three consecutive appointments. Patients in ASA 3 and 4 category should be rechecked in 5 minutes and if it is still elevated, immediate medical consultation is recommended.
- ASA 1 : BP less than 140/90.
- ASA 2 : BP 140-159 and/or 90-94.
- ASA 3 : BP 160-199 and/or 95-114.
- ASA 4 : BP more than 200 and/or more than 115.
*Normal BP values in younger patients are lower than those in adults.
Heart rate and rhythm
Heart rate (pulse) and rhythm can be measured through palpation of any readily accessible artery.
- Brachial artery, located on the medial aspect of the antecubital fossa.
- Radial artery, located on the radial and volar aspects of the wrist.
- Carotid artery : Should be palpated in emergency situations, as it delivers oxygenated blood to the brain.
- Femoral artery : Not frequently used as it not much accessible
Clinical guidelines
-
When palpating for a pulse, the doctor should press the index and middle fingers onto the patient's skin gently enough to feel the pulsation but, not so firmly that the pressure occludes the artery.
-
Thumb should not be used as it has a relatively large artery that pulsates. There are cases where the recorded heart rate is of the doctor, not the patient.
-
In infants, brachial artery in the upper arm is the preferred site.
-
The following factors are to be recorded during palpation :
- Heart rate, recorded as beats per minute.
- Heart rhythm, regular or irregular.
- Pulse quality (thready, strong, bounding or weak).
Heart Rate
- Should be evaluated for a minimum of 30 seconds, ideally for 1 minute.
- Normal resting heart rate in adults : 60-110 beats per minute. Bradycardia is less than 60 and tachycardia is more than 110.
- Heart rate is lower in well-conditioned athletes and elevated in apprehensive patients.
Heart rhythm
- Normal heart maintains a relatively regular rhythm known as normal sinus rhythm (NSR).
Premature Ventricular Contraction (PVC)
- Represents contraction of the ventricles (esp. left ventricle) before enough blood volume is present in their chambers to produce a pulse wave in a peripheral artery.
- These are detected clinically as breaks in a generally regular heart rate in which a longer than normal pause (e.g., "my heart skipped a beat") is noted and followed by resumption of normal rhythm.
- Occasional PVCs are common and not necessary considered abnormal. However, when PVCs are present at a rate of five or more per minute in patient with other risk factors or coronary artery disease, medical consultation should be considered.
- Provoking factors : Smoking, fatigue, stress, medications such as epinephrine and alcohol.
- Patient with frequent PVC are considered to be candidates for implanted cardioverter/defibrillators.
Pulsus alternans
- It represents a regular heart rate characterised by a pulse in which strong and weak beats alternate, caused by alternating contractile force of a diseased left ventricle.
- Observed frequently in left ventricular failure, severe arterial high blood pressure and coronary artery disease, and medical consultation is recommended.
Pulse quality
- The quality of pulse is commonly described with adjectives that relate to the subjective feel of the pulse, and can be described as bounding, thready, strong or weak.
- Very high blood pressure : Strong, bounding pulse.
- Hypotension and shock : Weak and thready pulse.
Respiratory rate
It must be assessed surreptitiously i.e., in a way that avoids attention of the patient, since the patient aware of the assessment usually do not breathe normally.
- After the heart rate is recorded, the doctor should keep their fingers on the patient's radial or brachial pulse and count respirations by observing the rise and fall of the patient's chest for a minimum of 30 seconds (ideally for 1 minute).
- Normal adult respiratory rate : 16-18 breaths per minute. It is more in young children.
- Bradypnea (slow respiratory rate) may be produced by opioid administration, while tachypnea (rapid respiratory rate) is seen with fever and alkalosis.
Temperature
It should be monitored orally, if possible.
- The thermometer, sterilised and shaken down, is to be placed under the tongue of the patient and mouth is closed for 2 minutes before removal.
- The patient should not eat, smoke or drink anything 10 minutes before the recording.
Clinical guidelines
- Normal oral temperature : 37o C (98.2o F) or 36.1o-37.5o C (97o to 99.6o F).
- Body temperature varies slightly throughout the day (0.25o-1.1o C or 0.5o-2.0o F), it is lowest in the early morning and highest in the late afternoon.
- Temperature above 38.3o C (101o F) : Usually indicate the presence of an active pathologic process.
- Temperature above 40o C (104o F) : Elective dental care is contraindicated and medical consultation is suggested.
References
-
Medical Emergencies in the Dental Practice (7th Edition), Stanley F. Malamed, Daniel L Orr II, Mosby Elsevier.
-
The image used is made available under the Creative Commons CCO 1.0 Universal Public Domain Dedication.
*This article is an excerpt from the above mentioned book and Medical Sutras does not make any ownership or affiliation claims.