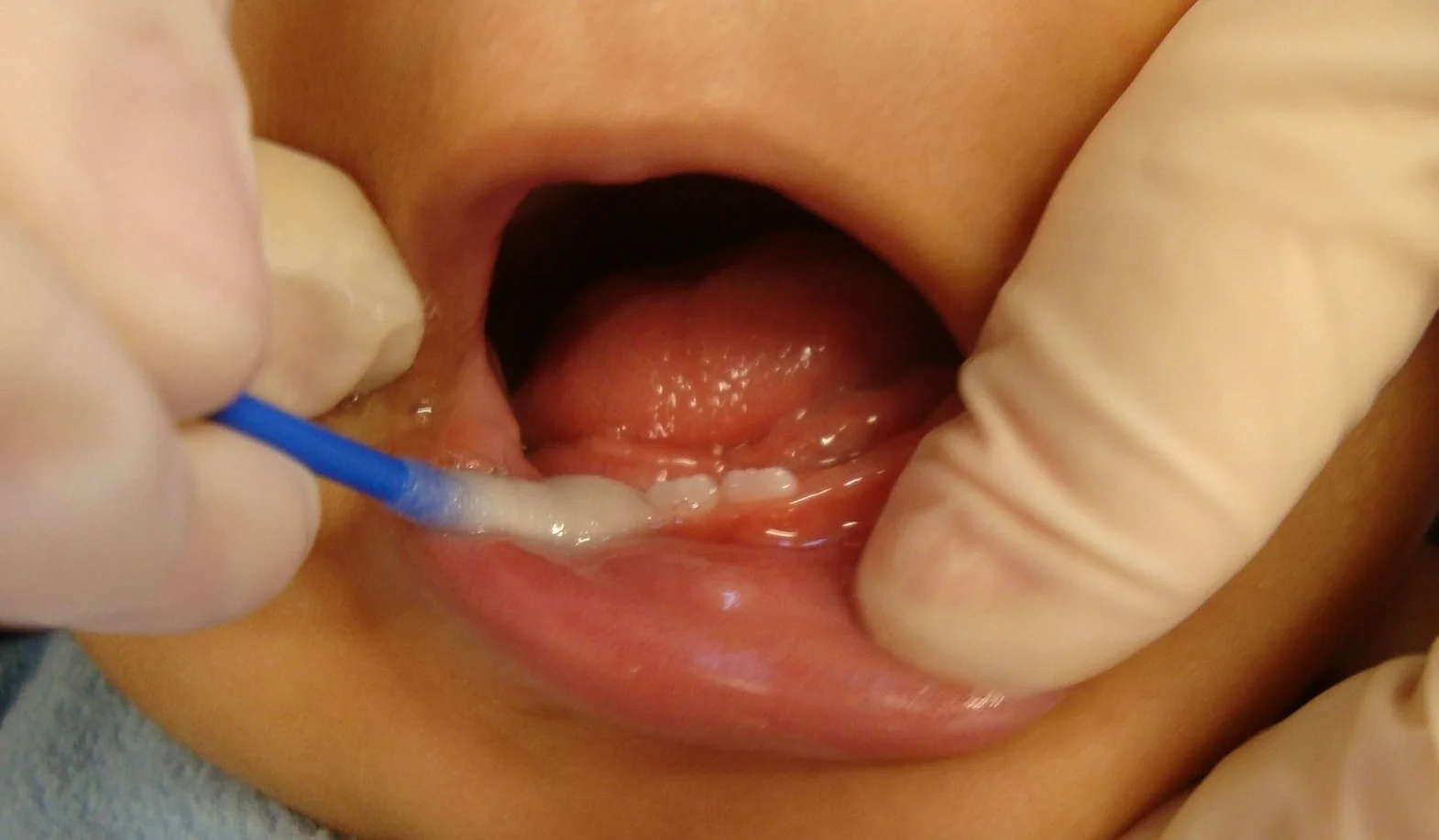
Topical fluoride therapy refers to the topical or local application of relatively large concentrations of fluoride to the erupted tooth surface to prevent the formation of dental caries.
Rationale
The enamel is not completely calcified at the time of tooth eruption and it continues calcification during the post-eruptive period (enamel maturation period) for approximately 2 years.
- During this period, the enamel acquires fluoride rapidly, as it is porous and immature immediately after eruption.
- Fluoride derived from saliva and from exposure to fluoride-containing water and food deposits in the superficial layer of enamel.
- Hence, the application of topical fluorides immediately after eruption can hasten fluoride uptake and makes enamel more resistant to dental caries.
Mechanism of Action
- Most topical fluoride agents have a fluoride ion concentration of between 10,000-20,000 ppm which leads to the formation of calcium fluoride and eventually fluorhydroxyapatite crystals.
- Ca10[PO4]6[OH]2 + 20F- -> 10CaF2 + 6[HPO4-]3 + 2[OH]-
- Fluoride ions have greater bonding potential and when substituted into the hydroxyapatite crystals fit more perfectly than hydroxyl ions. This makes the apatite crystal more compact and more stable, resulting in increased resistant to the acid dissolution.
The efficacy of topical fluoride depends on:
- Concentration of fluoride used.
- Frequency and duration of application.
- Specific fluoride compound used.
Classification
Professionally Applied Topical Fluorides
-
Aqueous solutions
- Sodium fluoride (2%, 9,200 ppm F).
- Stannous fluoride (8%, 19,500 ppm F).
-
Fluoride gels
- Acidulated phosphate fluoride (1.23%, 12,300 ppm F).
-
Fluoride varnishes
- Duraphat.
- Fluorprotector.
-
Fluoride prophylactic paste.
-
Restorative material containing fluoride.
-
Fluoride containing devices (slow release).
Self Applied Topical Fluorides
- Fluoride dentifrices.
- Fluoride mouth rinses.
Indications
Professionally applied topical fluorides are indicated in:
- Patients at high risk for smooth surface caries and root surface caries.
- Reduction in tooth sensitivity.
- White spot lesions.
- Active caries.
- Special patient groups such as, orthodontic patients, patients undergoing head and neck irradiation and patients with decreased salivary flow.
- Children whose permanent molars should, but cannot be sealed.
- Additional protection for children in areas without fluoridated drinking water (if necessary).
Advantages
- Does not cause fluorosis.
- Cariostatic for people of all ages.
- Available only to people who desire it.
- Easy to use.
Disadvantages
- Person must remember to use.
- Per capita cost is high, compared to water fluoridation.
- Short-term side effects like nausea may occur immediately after use of more concentrated professional use products.
References
- C. M. Marya - A Textbook of Public Health Dentistry, Jaypee Brothers Medical Publishers (P) Ltd (2011). https://amzn.to/3SHP36G
- S. S. Hiremath - Textbook of Public Health Dentistry, Elsevier India (2016). https://amzn.to/49mh2jw
- The image used is licensed under the Creative Commons Attribution-Share Alike 3.0 Unported. Source: Wikimedia Commons (Author: Odontoped-Ata).
*This article is an excerpt from the above mentioned books and Medical Sutras does not make any ownership and affiliation claims.