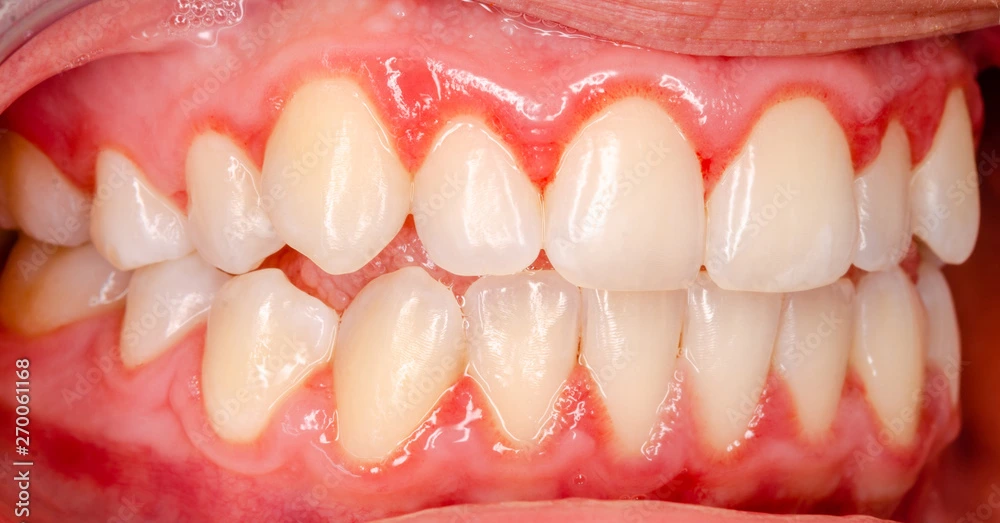
Gingivitis refers to the inflammation of gingiva. The main causative factor is dental plaque (plaque microorganisms are responsible for the pathological changes in gingivitis).
Stages of Gingival Inflammation
- Initial
- Early
- Established
- Advanced
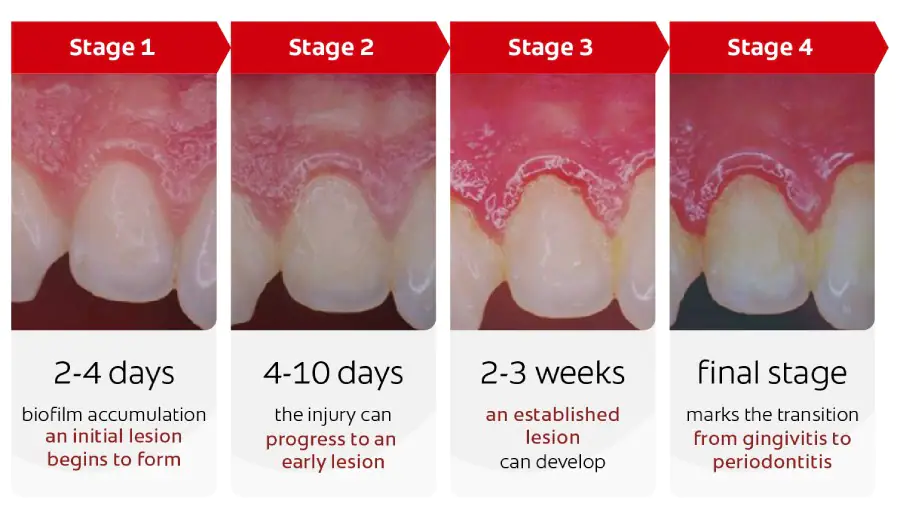
Image Source: https://www.colgateprofessional.com/students-faculty/trending-topics/can-you-take-a-vacation-from-oral-care
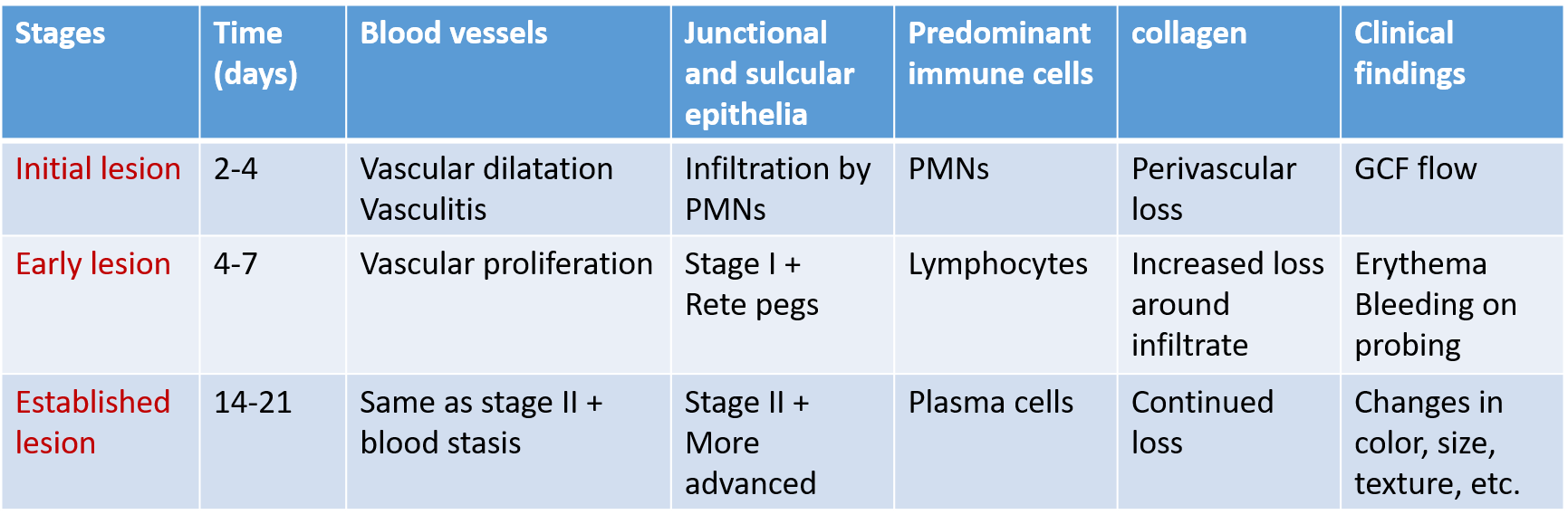
Stage I: The Initial Lesion
The initial response of gingiva is clinically not apparent. Hence, it is called subclinical gingivitis. Vascular changes are the first manifestation of gingival inflammation.
Clinical Manifestations
- Vascular changes: Dilated capillaries and increased blood flow.
- The vascular changes are due to microbial activation of leukocytes and subsequent stimulation of endothelial cells.
- Perivascular connective tissue matrix becomes altered.
- Exudation and deposition of fibrin in the affected area.
- Increase in GCF flow.
Microscopic Features
(Seen in connective tissue beneath junctional epithelium)
- Blood vessel morphology: Widening of small capillaries.
- Margination: Adherence of neutrophils to the vessel wall (occur in 1 week).
- Diapedesis (Emigration): PMNs leave the capillaries by migrating through the walls.
- PMNs can be seen in increased quantities in the connective tissue, the junctional epithelium and the gingival sulcus.
- Exudation of fluid from the gingival sulcus.
Stage II: The Early Lesion
It is called early gingivitis because of the presence of clinical signs of inflammation, and, occurs 1 week after the beginning of plaque accumulation.
Clinical Manifestations
- Erythema, due to proliferation of capillaries and increased formation of capillary loops between rete pegs and ridges.
- Bleeding on probing.
- Increase in GCF flow.
Microscopic Features
- Leukocyte infiltration: Seen in the connective tissue beneath the junctional epithelium, consisting mainly of lymphocytes (T cells) and neutrophils, as well as macrophages, plasma cells and mast cells.
- Increased transmigration of leukocytes in 6-12 days.
- Phagocytosis: PMNs are attracted to bacteria and engulf them in the process of phagocytosis.
- PMNs leave the blood vessel -> Follow the chemotactic stimuli from plaque bacteria -> Travel to epithelium -> Cross the basement membrane -> Reach the gingival sulcus.
- The amount of collagen destruction increases (70%).
- The main fibers affected are circular and dentogingival fiber groups.
- Fibroblasts show cytotoxic alteration with increased capacity to collagen production.
Stage III: The Established Lesion
Some established lesion remain stable, do not progress for months or years, while, others are more active and convert to progressively destructive lesions.
Clinical Manifestations
- Blood vessels become engorged and congested, venous return is impaired, and the blood flow becomes sluggish.
- The result is localized gingival anoxemia which superimposes a somewhat bluish hue on the reddened gingiva.
- Deepening of the color of gingiva is due to the extravasation of erythrocytes into connective tissue and the breakdown of hemoglobin.
Microscopic Features
- An intense, chronic inflammatory reaction is seen.
- Increased number of plasma cells (key feature). Plasma cells invade deep into the connective tissue, around blood vessels and between bundles of collagen fibers.
- Predominance of B lymphocytes (immunoglobulin G1 and G3).
- Junctional epithelium presents widened intercellular spaces filled with lysosomes. The lysosomes contain acid hydrolases that can destroy tissue components.
- Rete pegs or ridges protrude into the connective tissue, and the basal lamina is destroyed in some areas.
Other Findings
- Increased collagenolytic activity (due to collagenase enzyme).
- Increased levels of acid and alkaline phosphatase, beta-glucuronidase, beta-glucosidase, beta-galactosidase, esterase, aminopeptidase and cytochrome oxidase.
Stage IV: The Advanced Lesion
The lesion extends into the alveolar bone and is characterised by periodontal breakdown
Microscopic Features
- Fibrosis of gingiva.
- Widespread inflammatory and immunopathologic tissue damage.
- Plasma cells continue to dominate the connective tissue, and neutrophils continue to dominate the junctional epithelium and gingival crevice.
Important Points
- Sluggish: A marked slow movement or flow.
- Anoxemia: Abnormally low oxygen content in arterial blood.
- Collagenase: An enzyme normally present in gingival tissue and is produced by some oral bacteria and by PMNs in inflammatory conditions. It destroys the collagen by breaking the peptide bonds in it.
- With good periodontal therapy, stage III gingivitis appears to be reversible.
- Stage IV is irreversible because it involves the breakdown of alveolar bone.
References
- Newman and Carranza's Clinical Periodontology (11th edition), Elsevier, https://amzn.to/49PAzIx
- The image used in the cover photo is available on Adobe Stock, https://stock.adobe.com/search?k=gingivitis&asset_id=270061168.
*This article is an excerpt from the above mentioned book and Medical Sutras does not make any ownership or affiliation claims.