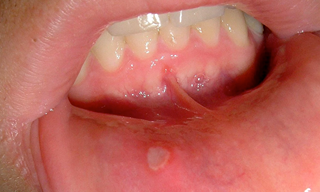
Recurrent Aphthous Stomatitis (RAS) is characterised by recurring ulcers confined to the oral mucosa with no other associated disease. It is considered a diagnosis of exclusion where the ulcers cannot be attributed to any other etiology.
Etiology
The cause of RAS is not certain, however, the following are frequently associated with RAS :
-
Bacterial Infection : Immunologic hypersensitivity to L-form of alpha Streptococcus and Streptococcus sanguis (T-cell mediated cross-reaction between streptococcal heat shock protein and oral mucosa).
-
Genetic Predisposition : Human Leukocyte Antigens (such as HLA-B51) have been identified in RAS patients.
-
Immunologic abnormalities : Local immune response against antigenically altered mucosa.
-
Nutritional Deficiency, particularly serum iron, folic acid and Vitamin B12.
-
Hormonal Disturbances : Related to progesterone levels.
-
Local trauma to the oral mucosa.
-
Anxiety and periods of psychological stress.
-
Allergic factors such as food allergy.
-
Upper respiratory tract infections.
-
Systemic diseases :
- Cyclic neutropenia.
- Magic Syndrome (Major aphthous and Generalised inflammed cartilage).
- PFAPA Syndrome (Periodic fever, aphthae, pharyngitis and cervical adenitis).
- Celiac disease (Autoimmune, intolerance to gluten).
- HIV Infection.
Classification
- Recurrent Aphthous Minor (Canker sore).
- Recurrent Aphthous Major (Mikulicz's scarring aphthae or Sutton's disease)
- Recurrent Herpetiform Ulcerations.
- Recurrent Ulcers associated with Bechet's Syndrome.
Recurrent Aphthous Minor
- Most common type.
- Ulcers are shallow, rounded, 3-7mm in diameter, with a sharply defined erythematous margin in the initial stage. The margin reduces once the lesion reaches its full size, and becomes irregular or lost as it heals.
- Commonly found in non-keratinised mucosa such as buccal and labial mucosa, buccal and lingual sulci, tongue, soft palate, pharynx and ginigiva.
- Sequence of Events : Begins with prodromal burning 24-48 hours before an ulcer appears, followed by a localised area of erythema. After few hours, a small white papule forms, ulcerates and gradually enlarges over the next 48-72 hours. The lesion persists for 7-14 days, followed by gradual healing with little or no scarring.
Recurrent Aphthous Major
- Most severe form, extremely painful and interfere with speech and eating.
- More common in patients with HIV infection.
- The ulcers may exceed 1 cm in diameter and heals slowly.
- May last for months and leave scar upon healing.
- They recur in waves over a long period of time.
Recurrent Herpetiform Ulcers
- Least common type, measuring less than 5mm (1-2mm).
- Occur in crops of multiple small, swallow ulcers, upto 100 in numbers.
- Usually seen in the floor of mouth and ventral tongue.
Laboratory Findings
-
Early lesions demonstrate an infiltration of large granular lymphocytes and helper CD4 lymphocytes with focal degeneration of basal cells and formation of small intraepithelial vesicles.
-
Anitschkow cells : Cells with elongated nuclei containing a linear bar of chromatin with radiating processes of chromatin extending towards nuclear membrane.
-
Biopsies reveal a superficial ulcer covered by a fibrinous exudate with granulation tissue at the base and mixed acute and chronic inflammatory infiltrate.
-
Laboratory tests are helpful to identify :
- Haematological deficiencies eg. low serum levels of vitamin B12, folate, ferritin and iron.
- HIV patients with CD4 count below 100/mm3.
Treatment
Tetracycline (0.25%) or Minocycline (0.2%)
- Swish and spit : To be held in mouth for 2-3 minutes, 3-4 times daily.
- Significantly reduces frequency and severity of the lesions.
- Best suited for herpetiform aphthae.
- Dosage : Tetracycline - capsule (250mg in 180 ml water) or syrup (250mg/5ml), Minocycline - 100mg tablet in 180ml water.
Chlorhexidine (0.2%)
- Three times daily after meals, to be held in mouth for at least 1 minute.
- Claimed to reduce the duration and discomfort.
Topical Anesthetics (for pain control)
- Benzocaine (10%) or 2% viscous lidocaine : Applied to the affected site, 3-4 times a day.
- Benzydamine hydrochloride (0.15%) : Swish and spit, 5-15ml, 3-4 times a day.
Topical Immunosupressants
- Applied to the affected site 3-4 times in a day, with no drink or food intake for 20-30 minutes afterward.
- 1.5% cortisone acetate gel.
- Hydrocortisone acetate (2.5mg) tablets : allowed to dissolve in the mouth, next to the ulcer, 3 times a day.
- Triamcinolone (0.1%) in methylcellulose paste.
- Dexamethasone elixir (0.5mg/5ml).
- Clobetasol (0.05%) gel
- Betamethasone (0.05%) gel
- Fluocinolone (0.05%) gel
- High-potency topical steroids are preferred in severe cases.
Amlexanox (5%) : Immunomodulatory prescription medicine with anti-inflammatory properties, has shown some effectiveness.
Intralesional steroids
- Can be used to treat large and recalcitrant major RAS lesions.
- Triamcinolone injections at 5-10 mg/cm2 of ulceration.
Systemic Therapy
- For severe cases that do not respond to topical agents.
- Predinsolone (1mg/kg), Pentoxifylline, Dapsone, Colchicine, Azathioprine, Thalidomide.
Points to Note
-
Nicotine metabolites are believed to decrease the level of proinflammatory cytokines and increase anti-inflammatory cytokines. Hence, the incidence of RAS is significantly lower among smokers.
-
Laboratory tests should be ordered when patients do not follow the usual pattern of RAS eg. when the episodes become more severe, begin past the age of 25 years or are accompanied by other signs and symptoms.
-
Biopsies are indicated only when it is necessary to exclude other diseases, such as Crohn disease, sarcoidosis, pemphigus or pemphigoid.
-
Anitschkow Cells are also found in
- Sickle cell anemia
- Megaloblastic anemia
- Iron deficiency anemia
- Children receiving chemotherapy for cancer
-
The steroid gel can be applied directly over the ulcers after meal and at bedtime, 2-3 times daily, while in case of larger lesions, a gauze containing the topical steroid can be placed and left for 15-30 minutes to allow longer contact of the medication.
-
Tetracycline is not indicated in pregnant women, since it can cause tooth discoloration.
-
Thalidomide is associated with severe, deforming and life-threatening birth defects, hence should be used with extreme caution in pregnant women. In the United States, clinicians prescribing thalidomide must be registered in the Risk Evaluation and Mitigation Strategy (REMS) program for thalidomide.
References
-
Burket's Oral Medicine, 13th Edition, Michael Glick, Martin S. Greenberg, ,Peter B. Lockhart, Stephen J. Challacombe, Wiley Blackwell.
-
Shafer, Hine, Levy Shafer's Textbook of Oral Pathology (7th Edition), Editors - R Rajendran, B Sivapathasundharam, Elsevier.
-
Cawson's Essentials of Oral Pathology and Oral Medicine, 9th Edition, EW Odell, Elsevier.
-
Contemporary Oral Medicine, A Comprehensive Approach to Clinical Practice, Camile S Farah, Ramesh Balasubramaniam, Michael J Mccullough, Springer.
-
Anil Govindrao Ghom, Savita Anil Ghom (Lodam) - Textbook of Oral Medicine - Jaypee Brothers Medical Publishers (P) Ltd (2014).
-
The image used is licensed under the Creative Commons Attribution-Share Alike 4.0 International license.
- Description : Mouth Ulcer. This is an edited version of the source image made for use in the "Anatomist" iOS and Android app and shared here under the terms of the source image's Share Alike Creative Commons license.
- Source : https://commons.wikimedia.org/wiki/File:Aphthe_Unterlippe.jpg.
- Author : Maksim.
*This article is an excerpt from the above mentioned books and Medical Sutras does not make any ownership or affiliation claims.