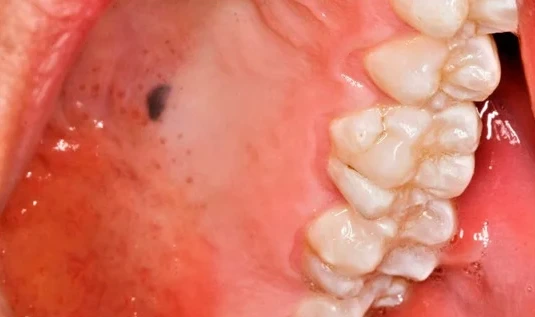
Nevi are benign proliferations of nevus cells in either epithelium or connective tissue, categorised as hamartomas, developmental malformations.
Synonyms: Oral melanocytic nevus, Nevocellular nevus, Mucosal melanocytic nevi.
Evolution: Both oral and skin nevus evolve from junctional nevus to intradermal nevus.
- Junctional nevi are first noted in infants, children and young adults and typically matures into compound nevi.
- During later adulthood, the lesions mature into intramucosal nevi.
- As the nevus cells penetrate into the dermis, their pigmentation diminishes and approximately 15% of intramucosal nevi are nonpigmented.
Classification
Nevi can be classified as congenital or acquired (Buchner and Hansen).
Based on histologic location of the nevus cells, cutaneous acquired nevi can be classified into three categories:
- Junctional nevus: Nevus cells are limited to the basal cell layer of the epithelium.
- Compound nevus: Nevus cells are in the epidermis and dermis.
- Intradermal nevus (Common mole): Nests of nevus cells are entirely in the dermis.
*Oral nevi follow the same classification where the term intradermal is replaced by intramucosal.
Ainsworth and Colleagues: Divided congenital nevi of the skin into small and garment nevi.
- Small nevi: Greater than 1 cm in diameter (usually 3-5cm).
- Garment nevi: Greater than 10 cm in diameter and can cover large areas of skin.
Clinical Features
The most common mucosal type is the intramucosal nevus, that accounts for more than one half of all reported oral nevi. The blue nevus is the second most common type found in the oral cavity (25-36%). Junctional and compound nevi account for only 3-6% of all oral nevi.
Intradermal Nevus
- May be a smooth flat lesion or may be elevated above the surface.
- May or may not exhibit brown pigmentation.
- Often shows strands of hair growing from its surface.
- Seldom occurs on the soles of the feet, the palms of the hands or the genitalia.
Junctional Nevus
- Clinically may appear similar to the intradermal nevus.
- Distinction is chiefy histologic and extremely important, since, the prognosis of the two lesions is different.
Compound Nevus
- Composed of two elements: an intradermal nevus and an overlying nevus.
Spindle cell/Epithelioid cell nevus (Spitz nevus)
- Occurs chiefly in children, only about 15% in adults.
- Adult lesion may appear histologically similar to malignant melanoma.
- Essentially, the lesion is clinically benign, but histologically malignant.
- Not reported on mucous surface, incl. the oral cavity.
Blue Nevus
- True mesodermal structure composed of dermal melanocytes which only rarely undergo malignant transformation.
- Occurs chiefly on the buttocks, on the dorsum of the feet and hands, on the face and occasionally on other areas.
- The lesion is smooth, exhibits hairs growing from its surface and varies in color from brown to blue or bluish black.
Oral Manifestations
Most oral nevi are asymptomatic, usually detected as an incidental finding on routine dental examination.
-
Approximately 85% of oral nevi are pigmented, varies from brown to black to blue.
-
Well circumscribed, round or oval, and are raised or slightly raised in 65-80% cases.
-
Approx. 15% are amelanotic.
-
Anatomic distribution: Closely follows histologic type.
- Blue nevi: 2/3rd occur in hard palate.
- Intramucosal nevi are distributed almost equally between hard palate and buccal mucosa (25% in each location), 17% on the gingiva, 12% on the vermilion border of the lip and almost 9% on the labial mucosa.
Differential Diagnosis
Melanotic macules, Amalgam tattoos, physiologic ethnic pigmentation, smoker's melanosis, or other vascular or pigmented lesions.
- Majority of nevi elevate from the mucosal surface.
- Melanotic macules and amalgam tattoos are usually flat.
- Ethnic pigmentation: nearly always symmetric and rarely affects the surface topography or disturbs the normal stippling in the gingiva.
- Smoker's melanosis: Involves only the anterior gingiva and most often occurs in women who smoke and take oral contraceptives.
- Vascular lesions: Usually blanch with compression and aspiration may help in differentiation.
- Malignant melanoma: Frequently associated with diffuse areas of pigmentation, possible ulceration, nodularity, variegation in color and an irregular outline.
Histology
- Nevus cells are large, ovoid, rounded, or spindle-shaped cells with pale cytoplasm.
- May contain granules of melanin pigment in their cytoplasm.
- Nucleus is vesicular and lacks the dendritic processes typical of melanocytes.
- Melanosomes are retained by nevus cells and are not transferred to adjacent keratinocytes.
- They tend to be grouped in sheets or cords, called nest or thèque.
- Nevus cells also have the ability to migrate from the basal cell layer into the underlying connective tissue.
- Multinucleated giant nevus cells are seen sometimes, but are of little prognostic significance.
Intradermal Nevus
- The nevus cells are situated within the connective tissue and are separated from the overlying epithelium by a well defined band of connective tissue i.e., the nevus cells are not in contact with the surface epithelium.
Junctional Nevus
- Zone of demarcation is absent and the nevus cells contact and seem to blend into the surface epithelium.
- overlying epithelium is thin and irregular and shows cells apparently crossing the junction and growing down into the connective tissue, abtropfung or dropping off effect.
- This junctional activity has serious implications because junctional nevi have been known to undergo transformation into malignant melanomas.
Compound Nevus
- Shows features of both junctional and intradermal nevus.
- Nests of nevus cells are dropping off from the epidermis, while large nests of nevus cells are also present in the dermis.
Spindle cell/Epithelioid cell Nevus
- Commonly composed of pleomorphic cells of three basic types: spindle cells, oval or epithelioid cells and both mononuclear and multinucleated giant cells.
- The cells are arranged in well-circumscribed sheets and there is generally considerable junctional activity.
Blue Nevus
- Two types: Common blue nevus and cellular blue nevus.
- Common blue nevus: Elongated melanocytes with long branching dendritic processes lie in bundles, usually oriented parallel to the epidermis, in the middle and lower third of the dermis. There is no junctional activity. The melanocytes are typically packed with melanin granules, sometimes obscuring the nucleus, and these granules may extend into the dendritic processes.
- Cellular blue nevus: An additional cell type is present - A large, round or spindle cell with a pale vacuolated cytoplasm, commonly arranged in an alveolar pattern.
Treatment & Prognosis
- It has become customary to recommend removal of pigmented moles that occur in areas irritated by clothing such as the belt or collar line, or if they suddenly begin to increase in size, deepen in color or become ulcerated.
- It is well recognised that congenital nevi have a great risk for transformation to malignant melanoma.
- Surgical excision of all intraoral pigmented nevi is recommended as a prophylactic measure, because of the constant irritation of the mucosa in nearly all intraoral sites occasioned by eating, toothbrushing, etc.
References
- Shafer, Hine, Levy Shafer's Textbook of Oral Pathology (7th Edition), Editors - R Rajendran, B Sivapathasundharam, Elsevier.
*This article is an excerpt from the above mentioned book and Medical Sutras does not make any ownership or affiliation claims.