Necrosis is a form of cell death in which cellular membranes fall apart, and cellular enzymes leak out and ultimately digest the cell.
The substances released from dead cells leads to a local host reaction (inflammation), which helps to remove the debris and start the subsequent repair process.
Morphologic Changes
Necrosis is characterised by following cytoplasmic and nuclear changes:
Nucleus
It may show one of the following three patterns (due to breakdown of DNA and chromatin),
- Pyknosis : There is nuclear shrinkage and increased basophilia i.e, the nucleus condenses into a dark shrunken mass.
- Karyorrhexis : There is fragmentation of the pyknotic nucleus.
- Karyolysis : There is digestion of DNA by deoxyribonuclease (DNase), resulting in fading of basophilia and complete disappearance of the nucleus (in 1-2 days).
Cytoplasm
-
Increased eosinophilia, due to increased binding of eosin to denatured cytoplasmic proteins and loss of basophilic RNA in the cytoplasm.
-
May have a glassy, homogeneous appearance, mostly due to loss of lighter staining glycogen particles.
-
More prominent myelin figures.
-
Moth-eaten appearance, as the cytoplasm becomes vacuolated due to digestion of cell organelles by the enzymes.
-
Electron microscopic findings:
- Discontinuities in plasma and organelle membranes.
- Marked dilation of mitochondria associated with large amorphous intramitochondrial densities.
- Disruption of lysosomes.
- Intracytoplasmic myelin figures.
Mechanism and Fate of Necrosis
The mechanisms of necrosis vary with different types of injury. These include:
- Failure of energy generation (ATP) because of reduced oxygen supply or mitochondrial damage.
- Leakage of cellular contents including enzymes due to damage to cellular membranes such as plasma membrane and lysosomal membranes.
- Irreversible damage to cellular lipids, proteins and nucleic acids (may be caused by reactive oxygen species).
The necrotic cells may persist for some time or may be digested by enzymes and disappear.
- Dead cells may be replaced by myelin figures, that are either phagocytosed by other cells or further degraded into fatty acids. These fatty acids bind calcium salts, which may result in the dead cells ultimately becoming calcified.
- The enzymes responsible for digestion of the cell are derived from lysosomes, that may come from the dying cells themselves or from leukocytes recruited as part of the inflammatory reaction.
Types of Necrosis
Necrosis can be divided into several types based on the distinctive gross appearance, except for fibrinoid necrosis, which is detected only by histologic examination.
Coagulative Necrosis
- In coagulative necrosis, the affected tissues shows a firm texture and the underlying tissue architecture is preserved for at least several days after death of cells in the tissue (since the eosinophilic anucleate cells persists for days or weeks).
- This occurs most likely because the injury also denatures the enzymes (alongwith the structural proteins) and hence, blocks the proteolysis of the dead cells.
- Ultimately, the dead cells are digested by the lysosomal enzymes derived from the leukocytes recruited to the site of necrosis. The cellular debris is then removed by phagocytosis, mediated primarily by infiltrating neutrophils and macrophages.
- It is seen in infarcts (areas of necrosis caused by ischemia) in all solid organs, except the brain.
Liquefactive Necrosis
- The dead cells are completely digested and the affected tissue is transformed into a viscous liquid, that is eventually removed by phagocytes.
- It is seen in seen in focal bacterial (and sometimes fungal) infections, since the microbes stimulate rapid accumulation of inflammatory cells and the enzymes of leukocytes digest/liquefy the tissue.
- The material is frequently creamy yellow (called as pus), if there is acute inflammation, as in bacterial infections.
- For reasons unknown, liquefactive necrosis is also seen with the hypoxic death of cells within the CNS.
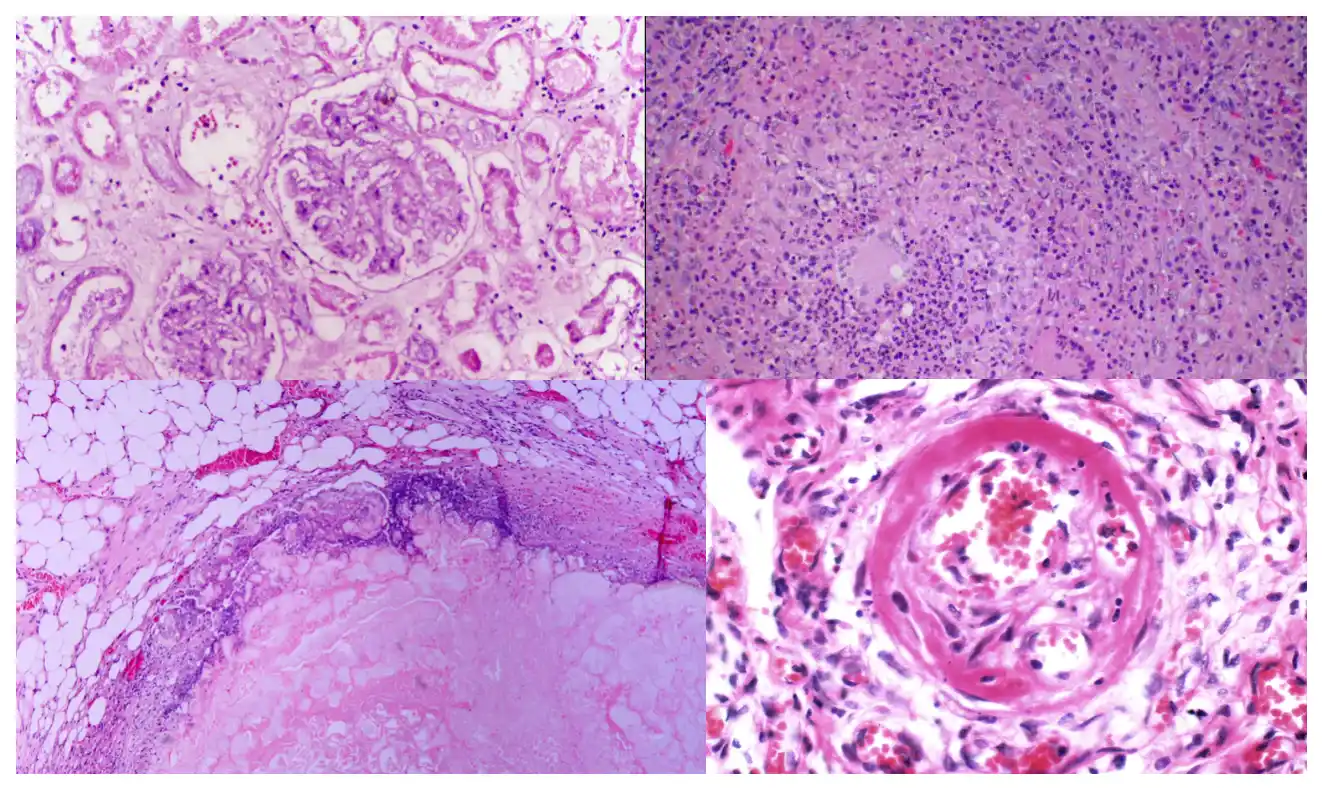
Caseous Necrosis
- In caseous necrosis, the tissue architecture is completely obliterated and cellular outlines cannot be discerned. The necrotic areas becomes cheeselike (friable yellow-white) in appearance, and hence the name caseous.
- Microscopic examination : Appears as a collection of fragmented or lysed cells with an amorphous granular pink appearance in H&E stain.
- It is often surrounded by a collection of macrophages and other inflammatory cells (this appearance is characteristic of granuloma, a nodular inflammatory lesion).
- It is most often encountered in foci of tuberculous infection.
Fat Necrosis
- It presents focal areas of fat destruction, that typically results from the release of activated pancreatic lipases into the substance of the pancreas and the peritoneal cavity.
- The released fatty acids combine with calcium to produce grossly visible chalky white areas (fat saponification).
- Histologic examination reveals shadowy outlines of necrotic fat cells surrounded by basophilic calcium deposits and inflammatory reaction.
Fibrinoid Necrosis
- It is a special form of necrosis that usually occurs in immune reactions (e.g., polyarteritis nodosa) in which antigen-antibody complexes are deposited in the walls of blood vessels.
- The deposited immune complexes and plasma proteins (leaked into the walls of damaged vessels) produce a bright pink, amorphous appearance on H&E stains, hence the name fibrinoid (fibrin-like).
- It may also occur in severe hypertension.
Points to Note
-
Tissue-specific necrosis can be detected using blood or serum samples as some proteins are specific to particular tissues and in the event of irreversible cell injury and cell death, these intracellular proteins leaks through the damaged cell membranes into the circulation. For example,
- Cardiac muscle contains a unique isoform of creatinine kinase and troponin.
- Hepatic bile duct epithelium contains the enzyme alkaline phosphatase.
- Hepatocytes contain transaminases.
Gangrenous Necrosis
- Refers to the condition of a limb (usually lower leg) that has lost its blood supply, resulting in coagulative necrosis of multiple tissue layers.
- It is not a distinctive pattern of necrosis, but still commonly used in clinical practice.
- Superimposition of bacterial infection leads to liquefactive necrosis (wet gangrene) due to the destructive bacterial contents and the attracted leukocytes.
References
- Robbins Basic Pathology, 10th edition, Vinay Kumar, Abul K. Abbas, Jon C. Aster, Elsevier.
- The images used are licensed under the Creative Commons license. Source: Wikimedia Commons.
*This article is an excerpt from the above mentioned book and Medical Sutras does not make any ownership or affiliation claims.