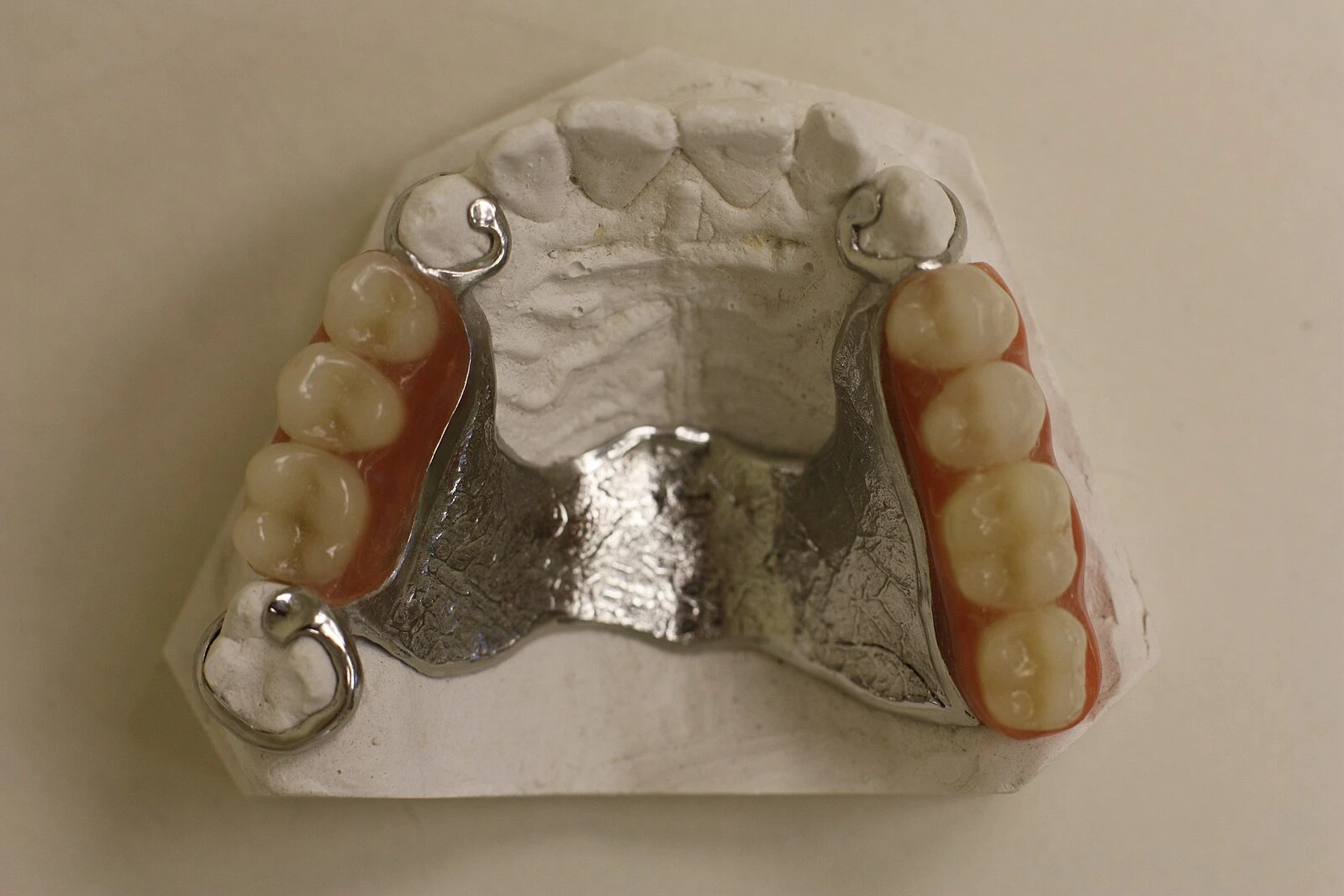
Based on the structure and design, the maxillary major connector are grouped as under :
- Single palatal strap.
- Combination anterior and posterior strap (Anteroposterior strap).
- Palatal plate.
- U-shaped palatal connector (Horseshoe connector).
- Single palatal bar.
- Combination anterior and posterior bar (Anteroposterior bar).
Single Palatal Strap
- It consists of a wide band of metal with minimum anteroposterior width not less than 8mm and a thin cross-sectional dimension.
- The strap can be made as wide as the combined width of a maxillary premolar and first first molar or the width can be increased as per the length of the edentulous space (to ensure rigidity and permit greater support from the hard palate).
- It should be confined within an area bounded by the four principle rests.
- Casting with a 22-gauge matte plastic pattern provides suitable rigidity without excessive bulk.
- Anterior border should be positioned posterior to the palatal rugae if possible, otherwise, it should be terminated on the posterior slopes of prominent rugae.
- Anterior border follows the valleys between rugae as nearly as possible, at right angles to the median suture line.
- Posterior border should be at right angle to the median suture line and positioned anterior to the junction of the hard and soft palates.
Indications
- Class III situations. (Bilateral tooth-supported short edentulous spaces, particularly, when the edentulous areas are located posteriorly.)
- May be used for unilateral distal extension partial dentures (Class II).
Advantages
- Can be made rigid without objectionable bulk.
- Little interference with normal tongue movement.
- Well accepted by patient.
- Applied stress is distributed over a large area due to increased tissue coverage.
- Offers great resistance to bending and twisting forces
Disadvantages
- Patient may complain of excessive palatal coverage (frequently due to improper positioning of strap borders).
- Should not be used to connect anterior replacements with distal extension bases, as there are chances of torque and leverage.
- Increased soft tissue coverage may predispose the patient to papillary hyperplasia. (Seen when the partial denture is worn 24 hours a day, accompanied by poor oral hygiene; may be due to inadequate patient instruction.)
Combination Anterior & Posterior Palatal Strap
- Each strap should be at least 8 mm wide and relatively thin in cross section.
- Borders should be kept 6 mm from the free gingival margins or should extend onto the lingual surfaces of the remaining teeth
- Palatal borders should exhibit smooth, gentle curves.
- The open area in the palatal region should be at least 20 x 15 mm.
Anterior Palatal Strap
- Anterior border not to be placed farther anteriorly than anterior rests and never closer than 6 mm to lingual gingival crevices.
- It should follow the valleys of the rugae at right angles to the median palatal suture.
Posterior Palatal Strap
- Posterior border should be located as far posterior as possible to avoid interference with tongue, but anterior to the junction of hard and soft palates (line of flexure).
- On the distal extension side, it is extended to hamular notch area.
- It should cross the median palatal suture at right angle.
- The posterior strap should not contact the tissues of the movable soft palate.
Lateral Palatal Straps
- 7-9 mm.
- Should be narrow and parallel to curve of arch, and located minimum of 6mm from gingival crevices of remaining teeth.
Indications
- Most frequently used in class II and IV arches.
- Class I and II arches in which excellent abutment and residual ridge support exists, and direct retention can be made adequate without the need for indirect retention.
- Presence of inoperable palatal tori, that do not extend posteriorly to the junction of hard palate and soft palate.
Advantages
- Structurally rigid, can be used in almost any maxillary palatal denture design.
- Flexure is practically nonexistent.
- Derives good support from the hard palate.
- Can be made relatively thin, as corrugated contour of the metal over the rugae adds strength to the connector
- Square or rectangular frame shape formed by joining of the anterior and posterior components provides a definite L-beam effect, thereby increasing the resistance to flexure.
Disadvantages
- Cannot be used in case of inoperable maxillary torus extending posterior to the soft palate.
- Interference with phonetics may occur in some patients.
- Extensive length of the borders may cause irritation to the tongue.
Palatal Plate Type Connector
Palatal plate is used to designate any thin, broad, contoured palatal coverage covering half or more of the hard palate.
- The anterior border must be kept 6 mm from the marginal gingiva or it must cover the cingula of the anterior teeth.
- Posterior border should extend to the junction of the hard and soft palates.
- The palatal plate should be located anterior to the posterior palatal seal area. The typical posterior palatal seal used in complete dentures, is not necessary because of the accuracy of cast metal.
- The portion contacting the teeth must have positive support from adequate rest seats.
Types
The palatal plate may be used in any one of three ways:
- As a palate of varying width that covers the area between two or more edentulous areas.
- As a complete or partial cast plate that extends posterior to the junction of the hard palate and soft palate.
- As an anterior palatal connector with a provision for extending an acrylic resin denture base in a posterior direction.
Indication
When the last remaining tooth on either side of a class I arch is the canine or first premolar tooth, especially when the residual ridges have undergone excessive vertical resorption.
Advantages
- It provides the ultimate support, as there is greatest amount of tissue coverage.
- A thinner casting can provide adequate rigidity and strength (due to corrugations in the anatomic replica).
- Uniformity in thickness and thermal conductivity makes the palatal plate more readily acceptable to the tongue and underlying tissue.
- Greater retention, by virtue of interfacial surface tension between metal and tissue due to intimate contact.
Disadvantage
- Increased cost
U-shaped Palatal Connector/Horseshoe Connector
- Consists of a thin band of metal running along the lingual surfaces of the remaining teeth and extending onto the palatal tissues for 6-8 mm.
- Medial borders should be placed at the junction of the horizontal and vertical slopes of the palate. They can be extended slightly onto the horizontal surfaces of the hard palate.
- The borders should be symmetric and extend to the same height.
- When it is used, indirect retainers must support any portion of the connector that extends anteriorly from the principle occlusal rests.
- All borders should be gently curved and smooth.
Indications
- Least desirable, from both the patient's standpoint and mechanical standpoint.
- Should be used only in situations in which inoperable tori extend to the posterior limit of the hard palate and occasionally when several anterior teeth are to be replaced.
Advantages
- Can derive some vertical support from tissues of the hard palate.
- Can be designed to avoid bony prominences without sacrificing vertical support (in the presence of prominent median suture line or inoperable torus).
Disadvantages
- It lacks rigidity (compared with other designs).
- Tendency to lateral flexure under occlusal forces, which may induce torque or direct lateral force on abutment teeth.
- The design fails to provide good support characteristics and may permit impingement of underlying tissue when subjected to occlusal loading.
- The metal crossing the anterior plane must be thicker to avoid tendency to flex, resulting in greater bulk and hinderance to tongue movement.
- Noticeable movement can occur at the open end and may result in concentration of forces and damage to the associated abutments.
- Poor choice for distal extension partial dentures.
- Not a good connector when cross-arch stability is required.
Single Palatal Bar
Narrow half oval shaped connector with its thickest point at the center and width less than 8 mm.
Indication
Should be avoided. Use limited to primarily in interim application, such as for short-span class III cases.
Disadvantages
- Least logical, often too thin and flexible or too bulky and objectionable to the patient's tongue.
- Its bulk may produce noticeable discomfort and alteration of speech, hence, should not be placed anterior to the second premolar position.
- Derives little vertical support from the bony palate.
- Must derive nearly all of its support from rests on the remaining teeth.
Combination Anterior & Posterior Palatal Bar
Displays characteristics of palatal bar and palatal strap major connectors.
Anterior Bar
- Relatively flat with cross-sectional shape similar to that of a palatal strap.
- Borders are positioned on the appropriate slopes of prominent rugae, thereby allowing it to bend with the contours of the anterior palate.
Posterior Bar
- Half oval in shape, similar to palatal bar.
- The two bars are joined by flat longitudinal elements on each side of the palate.
Indication
- When the anterior and posterior abutments are widely separated.
- Patients with large inoperable palatal tori.
Advantages
- The encirclement formed by joining of anterior and posterior components, provides considerably more rigidity than any of the individual elements.
- The two bars lying in different planes, produce a structurally strong L-beam effect.
- Minimum soft tissue coverage, yet provides exceptional resistance to deformation.
Disadvantages
- Exhibits many of the same disadvantages as the single palatal bar.
- Needs to be bulky to be sufficiently rigid and provide support and stability.
- Frequently uncomfortable: Bulk and contour may be bothersome to the tongue and may interfere with phonetics.
- Derives little support from the bony palate, due to limited contact with the palatal tissues.
- Contraindicated in patients with reduced periodontal support.
How to design maxillary major connectors?
Blatterfein (1953) recommended five basic steps in designing maxillary major connectors:
-
Outline of primary bearing areas: These areas will be covered by the denture base.
-
Outline of non-bearing areas: Includes the lingual gingival tissue within 5-6 mm of the remaining teeth, hard areas of the medial palatal raphe (including tori), and palatal tissue posterior to the vibrating line.
-
Outline of connector areas: Defined by taking into consideration the primary bearing and non-bearing areas,
-
Outline of connector type: Selection of the connector type is based on four factors :
- Mouth comfort.
- Rigidity.
- Location of edentulous ridge areas.
- Need for indirect retention.
-
Unification of the denture base areas and connectors.
Beading of the maxillary cast
Methodology
- Beading: Refers to the scribing of a shallow groove on the maxillary master cast outlining the palatal major connector exclusive of rugae areas.
- Bead lines: Refers to minor elevations on the maxillary major connector at the borders contacting the palatal soft tissues.
- The groove should not be larger than 0.5 mm in width or depth, and should fade out approximately 6 mm from the gingival margins of the remaining teeth.
- Can be created by scribing shallow channels on the surface of a cast before duplication in investment material.
- Instrumentation: Cleoid carver, small spoon excavator or round bur rotating at slow speed.
Purpose
- To transfer the major connector design to the investment cast.
- To provide a visible finishing line for the casting.
- To ensure intimate tissue contact of the major connector with selected palatal tissue, by slightly displacing the adjacent soft tissues. This enhances retention and stability of the denture, and produces a mechanical seal, that prevents collection of food particles under the major connector.
Points to Note
-
All maxillary major connectors should cross the midline at a right angle rather than diagonally. Tongue will accept symmetrically placed components far more readily than those placed without regard for symmetry.
-
All gingival crossing should be abrupt and at right angles to the major connector.
-
All borders should be tapered toward the tissue.
-
The tissue side of the major connector is not brought to a high finish during polishing procedures. (Electrolyte polishing is sufficient.)
-
Anterior border areas must be kept at least 6 mm away from adjacent teeth. If the anterior border contacts the remaining teeth, the connector must again be supported by rests placed in properly prepared rest seats.
-
Definite tooth support must be provided, whenever it is necessary for the palatal connector to make contact with the teeth for support: Best accomplished by establishing definite rest seats on the predetermined abutment teeth.
- These should be located far enough above the gingival attachment to provide for bridging of the gingival crevice with blockout.
- Also, they should be low enough on the tooth to avoid unfavourable leverage and incisal interference of the opposing dentition.
-
It should never be supported even temporarily by inclined lingual surfaces of anterior teeth.
-
L-beam principle: Forces transmitted on different planes are counteracted more easily.
References
- McCracken’s Removable Partial Prosthodontics (13th edition), Alan B. Carr DMD MS, David T. Brown DDS MS, Elsevier.
- Stewart’s Clinical Removable Partial Prosthodontics (4th edition), Rodney D. Phoenix, David R. Cagna, Charles F. DeFreest, Quintessence Books.
- The image used is licensed under the Creative Commons Attribution-Share Alike 3.0 Unported license. (Author : Sterilgutassistentin).
*This article is an excerpt from the above mentioned books and Medical Sutras does not make any ownership and affiliation claims.