Gastroesophageal reflux disease (GERD) involves the back flow of gastric acid and other gastric contents into the oesophagus.
- The normal anti-reflux mechanisms consist of the lower oesophageal sphincter, the diaphragm and the anatomical location of the gastro-oesophageal junction below the diaphragmatic hiatus.
- In healthy individuals, occasional episodes of gastro-oesophageal reflux are common. However, this is followed by cleaning of the gullet by oesophageal peristaltic waves and neutralisation of residual acid by alkaline saliva, that, results in no symptoms do not occur.
- GERD develops when the oesophageal mucosa is exposed to gastric contents for prolonged periods of time, resulting in the symptoms and in some cases, oesophagitis.
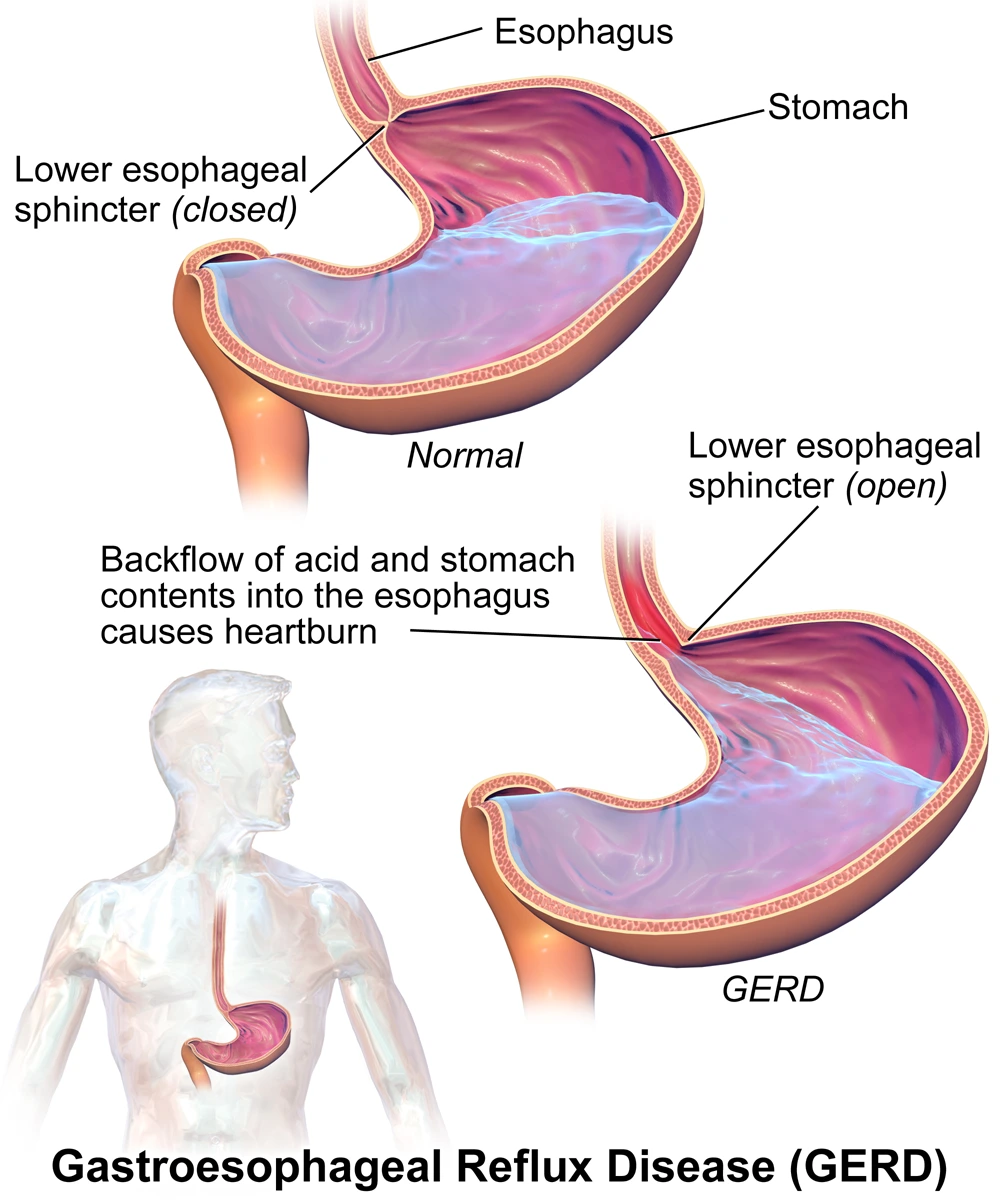
Etiology
Several factors, known to be involved in the etiology include,
-
Loss of gradient of pressure between the lower oesophageal sphincter and the stomach. This may occur due to muscle weakness (with no apparent cause) or lower oesophageal sphincter incompetence due to secondary causes, such as,
- scleroderma-like disease,
- myopathy associated with chronic intestinal pseudo-obstruction,
- pregnancy,
- smoking,
- anti-cholinergic drugs, smooth-muscle relaxants (beta adrenergic agents, aminophyline, nitrates, CCBs, phosphodiesterase inhibitors that increases cAMP or cGMP),
- surgical damage to LES and oesophagitis.
-
Increased gastric volume : After meals, in pyloric obstruction, in gastric stasis, during acid hyper-secretion states.
-
Close proximity of gastric contents near the gastro-oesophageal junction : In recumbency, bending down, hiatus hernia.
-
Increased gastric pressure : Obesity, pregnancy, ascites, tight clothes.
-
Incompetence of the diaphragmatic crural muscle.
-
Delayed oesophageal clearance with impaired salivary secretion (defective oesophageal peristaltic activity).
Clinical Features
- Characteristic symptoms : Regurgitation of sour materials in the mouth and heartburn. (Heartburn is produced by the contact of refluxed material with the sensitised or ulcerated oesophageal mucosa.)
- Reflux into the pharynx, larynx and tracheobronchial tree can cause chronic cough, bronchoconstriction, pharyngitis, laryngitis, bronchitis or pneumonia. Some patients are woken at night by choking as refluxed fluid irritates the larynx. Morning hoarseness may be noted.
- Recurrent pulmonary aspiration can cause aspiration pneumonia, pulmonary fibrosis or chronic asthma.
- Persistent dysphagia suggests development of peptic stricture. Most patients with peptic stricture have a history of several years of heartburn preceding dysphagia.
- A history of weight gain is common.
- Rapidly progressive dysphagia and weight loss may indicate the development of adenocarcinoma in Barrett's oesophagus.
- Angina-like or atypical chest pain occurs in some patients, while others experience no heartburn or chest pain. Many patients with GERD remain asymptomatic or self treated and do not seek attention until severe complications occur.
Complications
- Oesophagitis : It involves a range of endoscopic findings, from mild redness to severe bleeding ulceration with stricture formation.
- Barrett's oesophagus (columnar lined oesophagus or intestinal metaplasia of oesophagus) : It is a pre-malignant glandular metaplasia of the lower oesophagus, in which the normal squamous lining is replaced by columnar mucosa composed of a cellular mosaic containing areas of intestinal metaplasia. It occurs as a adaptive response to chronic gastro-oesophageal reflux, and is found in 10% of patients undergoing gastroscopy for reflux symptoms.
- Anaemia : Iron deficiency anaemia occurs as a consequence of of chronic, insidious blood loss from long-standing oesophagitis.
- Benign oesophageal stricture : Fibrous strictures develop as a consequence of long-standing esophagitis. Most patients are elderly and have poor oesophageal peristaltic activity. They present with dysphagia which is worse for solid than for liquids.
Diagnosis
-
Diagnosis can be made easily by history alone.
-
Diagnostic studies are indicated in patients with persistent symptoms or complications or those who do not respond to therapy.
-
The diagnostic approach to GERD can be divided into three categories :
- Documentation of mucosal injury.
- Documentation and quantitation of reflux.
- Definition of pathophysiology.
Documentation of mucosal injury
Mucosal damage is documented by the use of barium swallow, oesophagoscopy and mucosal biopsy.
- Barium swallow results are usually normal in uncomplicated oesophagitis but may reveal a stricture or ulcer (suggests Barrett's oesophagitis).
- Oesophagoscopy may reveal the presence of erosive oesophagitis, distal peptic stricture or columnar cell-lined lower oesophagus with or without a proximally located peptic stricture, or adenocarcinoma.
- Mucosal biopsy should be performed at least 5 cm above the LES, as the oesophageal mucosal changes of chronic oesophagitis are quite frequent in the most distal oesophagus in otherwise normal individuals.
Documentation and quantitation of reflux
- Documentation of reflux is necessary only when the role of reflux in the symptom complex is unclear, particularly in evaluation of supra-oesophageal symptoms and chest pain without endoscopic evidence of oesophagitis.
- It can be done by ambulatory long-term (24 hr) oesophageal pH recording.
Definition of pathophysiology
- Definition of pathologic factors in GERD is sometimes indicated for management decisions such as anti-reflux surgery.
Treatment
The goals of treatment are to provide symptom relief, heal erosive oesophagitis and prevent complications.
-
Management of mild cases include,
- Weight reduction, sleeping with the head of the bed elevated by about 4-6 inch with blocks and elimination of factors that increase abdominal pressure.
- Patient should not smoke and should avoid consuming fatty foods, coffee, chocolate, alcohol, mint, orange juice and certain medications (such as anticholinergic drugs, CCBs and other smooth muscle relaxants).
- Ingesting large amount of fluids with meals should also be avoided.
- Sodium alginate containing antacids, H2 blockers or PPIs are adequate.
-
Proton Pump Inhibitors (PPIs):
- Omeprazole (20 mg/d), Pantoprazole (40 mg/d), Rabeprazole (20 mg/d) for 8 weeks can heal erosive oesophagitis in upto 90% of patients.
- The drug is taken 15-30 min before breakfast and can be maintained indefinitely (Hit and Run drug).
- Aggressive acid suppression causes hypergastrinemia and also Vit B12 absorption is compromised by the treatment.
-
Patients who have Barrett's oesophagus with concomitant oesophagitis should be similarly treated. Patients who have an associated peptic stricture are treated with dilators to relieve dysphagia and such patients are provided with vigorous treatment for reflux.
-
Anti-reflux surgery (Fundoplication), in which the gastric fundus is wrapped around the oesophagus, increases the LES pressure and should be considered as an alternative for patients who require long term high dose PPIs.
- Ideal candidate are those in whom motility studies show persistently inadequate LES pressure but normal peristaltic contractions in the oesophageal body.
-
Patients with alkaline oesophagitis are treated with general anti-reflux measures and neutralisation of bile salts with cholestyramine, aluminium hydroxide or sucralfate.
References
- Harrison's Principles of Internal Medicine (17th edition), Fauci, Braunwald, Jasper, Hauser, Longo, Jameson, Loscalzo, The McGraw-Hill Companies.
- The image used as cover photo is licensed under the Creative Commons Attribution-Share Alike 3.0 Unported license (Source : SMART Servier Medical Art, part of Laboratories Servier.)
- The image used in the article is licensed Creative Commons Attribution-Share Alike 4.0 International license (Author : BruceBlaus, Source : Own work).
*This article is an excerpt from the above mentioned book and Medical Sutras does not make any ownership or affiliation claims