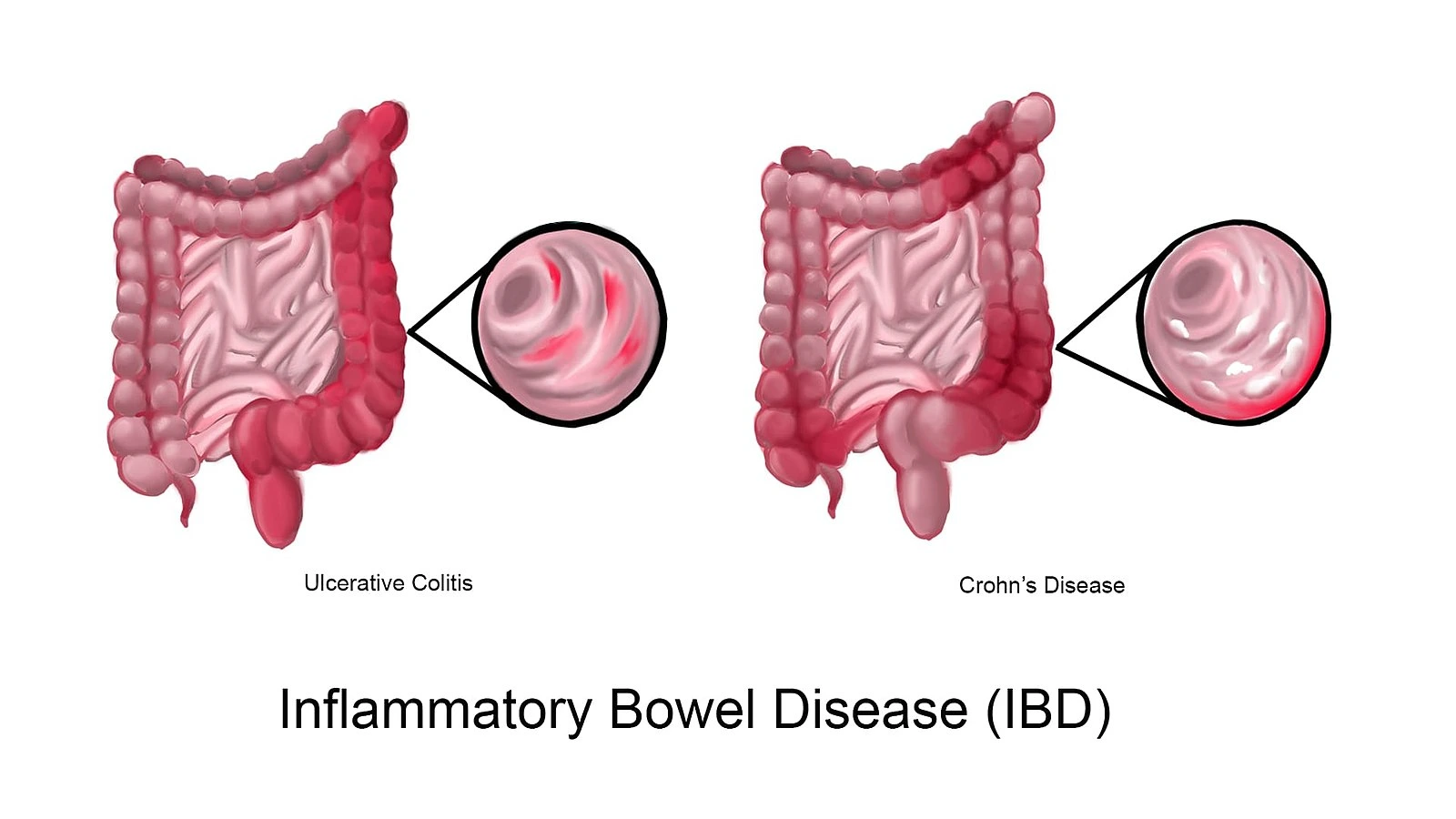
At least one extraintestinal disease is manifested in up to one-third of patients with Inflammatory Bowel Disease (IBD). The extra-intestinal manifestations include:
- Dermatologic: Erythema nodosum, Pyoderma gangrenosum, Pyoderma vegetans, Pyostomatitis vegetans, Sweet syndrome (neutrophilic dermatosis), Metastatic CD (Cutaneous granuloma formation), Psoriasis, Perianal skin tags, Oral mucosal lesions.
- Rheumatologic: Peripheral arthritis, Ankylosing spondylitis, Sacroiliitis, Hypertrophic osteoarthropathy, Pelvic/femoral osteomyelitis, Relapsing polychondritis.
- Ocular: Uveitis, Episcleritis, Conjunctivitis.
- Hepatobiliary: Hepatic steatosis (Fatty liver), Cholelithiasis (Gallstones), Primary sclerosing cholangitis (PSC).
- Urologic: Nephrolithiasis.
- Metabolic Bone Disorders: Low Bone Mass, Increased incidence of hip, sppine, wrist and rib fractures, Osteonecrosis.
- Venous and arterial thrombosis.
- Cardiopulmonary Manifestations: Endocarditis, Pleuropericarditis, Interstitial lung disease.
Dermatologic Manifestations
-
Erythema nodosum (CD - 15%, UC - 10%)
- Hot, red, tender nodules, 1-5 cm in diameter.
- Found on the anterior surface of the lower legs, ankles, calves, thighs, and arms.
- Develop after the onset of bowel disease and concomitant active peripheral arthritis is frequently seen.
- Treatment is directed toward the underlying bowel disease.
-
Pyoderma gangrenosum ( UC - 1-2%)
- Begins as a pustule and then spreads concentrically to rapidly undermine healthy skin. This is followed by ulceration, with violaceous edges surrounded by a margin of erythema. At the center, the lesions contain necrotic tissue with blood and exudates.
- Lesions may be single or multiple and grow as large as 30 cm.
- Usually presents after the diagnosis of IBD.
- Lesions are commonly found on the dorsal surface of the feet and legs (may occur on the arms, chest, stoma and even face).
- Sometimes very difficult to treat and often require IV antibiotics, IV glucocorticoids, dapsone, azathioprine, thalidomide, IV cyclosporine, infliximab or adalimumab.
-
Oral mucosal lesions : Aphthous stomatitis and cobblestone lesions of the buccal mucosa, seen often in CD (rarely in UC).
Rheumatologic Manifestations
-
Peripheral arthritis (15-20%)
- Asymmetric, polyarticular and migratory.
- Most often affects large joints of the upper and lower extremities.
- Worsens with exacerbations of bowel activity.
- Treatment: Reduce bowel inflammation. Severe UC: Colectomy frequently cures arthritis.
-
Ankylosing spondylitis (10%)
- Most often affects the spine and pelvis, producing symptoms of diffuse low-back pain, buttock pain and morning stiffness.
- Continuous and progressive in nature leading to permanent skeletal damage and deformity.
- 2/3rd IBD patients with ankylosing spondylitis express the HLA-B27 antigen.
- Not related to bowel activity, does not remit with glucocorticoids or colectomy.
- Anti-TNF therapy reduces spinal inflammation and improves functional status and quality of life.
-
Sacroiliitis
- Occurs equally in UC and CD.
- Often asymptomatic and does not correlate with bowel activity, does not always progress to ankylosing spondylitis.
Ocular Manifestations
-
Uveitis
- Symptoms: Ocular pain, photophobia, blurred vision and headache.
- May be found during periods of remission and may develop following bowel resection.
- Prompt intervention, sometimes with systemic glucocorticoids, is required to prevent scarring and visual impairment.
-
Episcleritis (3-4%)
- Benign disorder, presents with symptoms of mild ocular burning.
- Treated with topical glucocorticoids.
Hepatobiliary Manifestations
-
Hepatic steatosis (Fatty liver)
- Usually present with hepatomegaly.
- Results from a combination of chronic debilitating illness, malnutrition, and glucocorticoid therapy.
-
Cholelithiasis (Gallstones)
- Occurs in 10-35% of CD with ileitis or ileal resection.
- Caused by malabsorption of bile acids, resulting in depletion of the bile salt pool and secretion of lithogenic bile.
-
Primary sclerosing cholangitis (PSC)
- Characterised by both intrahepatic and extrahepatic bile duct inflammation and fibrosis, frequently leading to biliary cirrhosis and hepatic failure.
- 50-75% of patients with PSC have IBD.
- Most patients have no symptoms at the time of diagnosis, symptoms include fatigue, jaundice, abdominal pain, fever, anorexia and malaise.
- Traditional gold standard diagnostic test is Endoscopic Retrograde Cholangiopancreatography (ERCP), however, Magnetic Resonance Cholangiopancreatography (MRCP) is sensitive, specific and safer.
- Patients with gallbladder polyps have a high incidence of malignancy and cholecystectomy is recommended (even if the lesion is < 1 cm in diameter).
- Patients with IBD and PSC are at increased risk of colon cancer and should be surveyed yearly by colonoscopy and biopsy.
Urologic Manifestations
-
Nephrolithiasis (10-20%)
- Presents with Calculi, Ureteral obstruction and ileal bladder fistulas.
- Due to hyperoxaluria which results from increased absorption of unbound oxalate in the colon. (In ileal dysfunction, non-absorbed fatty acids bind calcium and leave oxalate unbound.)
Metabolic Bone Disorders
-
Low Bone Mass (14-42% cases)
- Risk is increased by glucocorticoids, cyclosporine, methotrexate and total parenteral nutrition.
- The effect of glucocorticoids id dose-dependent. Up to 20% of bone mass can be lost per year with chronic glucocorticoid use.
- Low bone density also occurs due to malabsorption and inflammation mediated by IL-1, IL-6, TNF and other inflammatory mediators.
-
Increased incidence of hip, sppine, wrist and rib fractures (CD- 36%, UC - 45%).
-
Osteonecrosis: Characterised by death of osteocytes and adipocytes and eventual bone collapse, seen in 4.3% patients within 6 months of starting glucocorticoids. Treatment consists of pain control, cord compression, osteotomy and joint replacement.
Thromboembolic disorders
-
Both venous and arterial thrombosis
-
Etiologic factors include:
- Abnormalities of platelet-endothelial interaction.
- Hyperhomocysteinemia.
- Alterations in coagulation cascade.
- Impaired fibrinolysis.
- Involvement of tissue factor-bearing microvesicles.
- Disruption of the normal coagulation system by autoantibodies.
- Genetic predisposition.
References
- Harrison's Principles of Internal Medicine (21st edition), Loscalzo, Fauci, Kasper, Hauser, Longo, Jameson, The McGraw-Hill Companies.
- The image used in the cover is licensed under the Creative Commons Attribution-Share Alike 4.0 International license. (Author : WolfpackBME, Source : Wikimedia commons).
*This article is an excerpt from the above mentioned book and Medical Sutras does not make any ownership or affiliation claims.