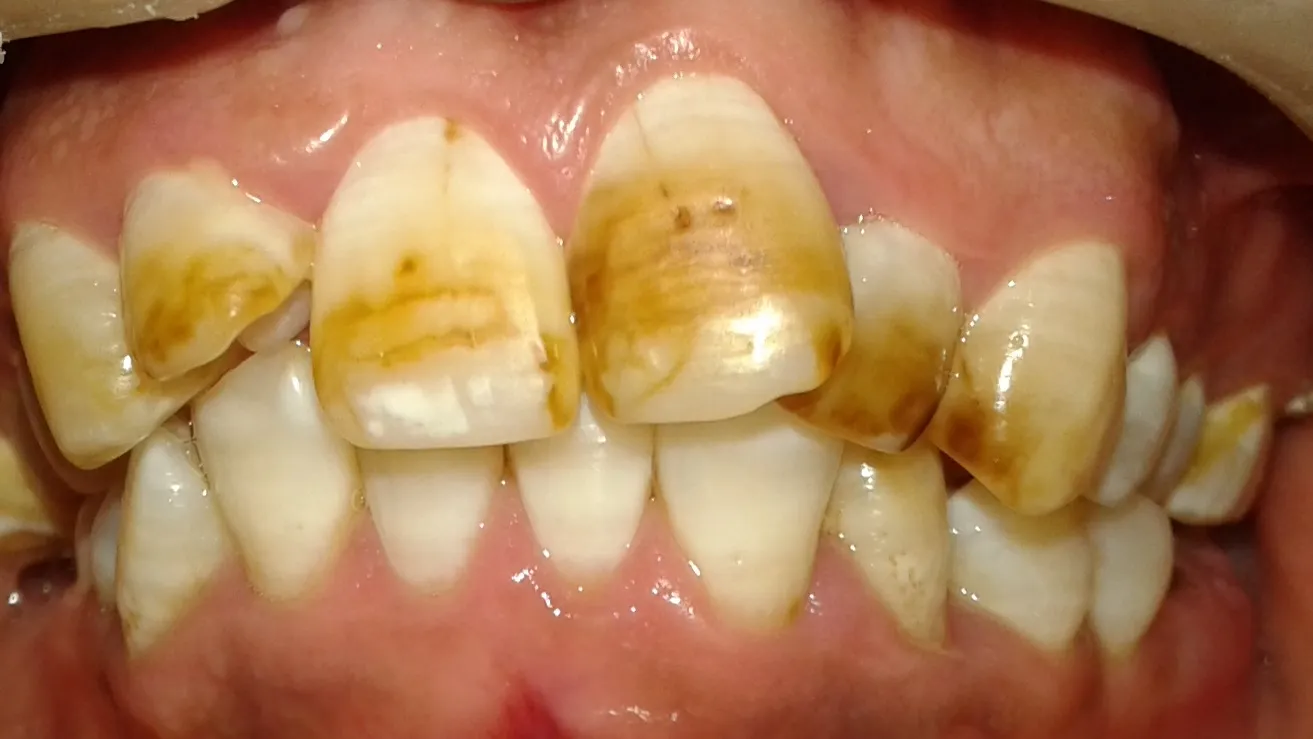
Dental fluorosis refers to hypoplasia or hypomineralization of enamel or dentin due to chronic intake of excessive amounts of fluoride during tooth development.
Factors Affecting the Severity and Distribution
- Fluoride concentration (dose dependent).
- Duration of exposure.
- Age of the subject.
- Individual susceptibility.
Pathophysiology
The definitive pathophysiology of dental fluorosis is not fully understood. However, it is believed that fluoride affects different phases of amelogenesis, thus, affecting enamel synthesis.
Critical Window Period: Birth to 8 years.
- High levels of fluoride in the plasma during this period results in formation of porous hypomineralized enamel, and the porosity can extend toward DEJ in severe cases.
- The most vulnerable stage is early maturation phase which gets delayed in fluorosed enamel.
- Fluoride has also been shown to induce apoptosis in ameloblasts during enamel maturation. It is believed that this contributes to the enamel pitting found in severe cases of dental fluorosis.
Clinical Manifestations
-
Mild form: Dull, opaque, white areas in the enamel.
-
Severe form: Mottled, discolored (yellowish brown to black stains) or pitted.
-
The discoloration may be in the form of spots or horizontal streaks.
-
Permanent teeth are more severely affected than primary teeth:
- Primary teeth undergoes most of the mineralisation before birth and placenta acts as a barrier against high concentrations of fluoride.
- Period of enamel formation is shorter in primary dentition.
- Enamel of primary teeth is thinner.
-
Most commonly affected primary tooth: Primary second molar.
Staging of Dental Fluorosis
There are multiple indices for staging of dental fluorosis. These are primarily used in epidemiological studies and include:
- Dean Modified Fluorosis Index.
- Thylstrup Fejerskov Index.
- Tooth Surface Index of Fluorosis.
- Fluorosis Risk Index.
Differential Diagnosis
Key points to recognise dental fluorosis:
- Positive fluoride history within the critical window of amelogenesis.
- Symmetrical chronological distribution pattern of affected teeth.
- Increased caries resistance.
Conditions:
- Incipient/Early caries.
- Molar-incisor hypomineralisation.
- Amelogenesis Imperfecta.
- Tetracycline staining.
- Turner hypoplasia.
- Dental manifestations of celiac disease.
*Incipient/Early Caries
- The tooth will be opaque, exhibiting no translucency due to the extensive subsurface porosity caused by demineralization.
- It may have a grayish-blue aspect of dentin beneath the enamel.
- White spot (incipient) lesion will disappear upon wetting, however, hypocalcification will remain whether dry or moist.
Management
Treatment of dental fluorosis is based on patient preferences and mostly involves cosmetic concerns.
Mild to Moderate Cases
- Patient may be unaware or not concerned with the aesthetics. In such cases, no treatment is required.
- Vital dental bleaching: Using hydrogen peroxide.
- Enamel microabrasion: Involves mechanically removing the superficial layers of fluorosed enamel to reduce the visibility of enamel discoloration.
- Resin infiltration: Involves etching the enamel with hydrochloric acid, followed by low-viscosity resin, which infiltrates the enamel.
- Resin-based dental composite such as localized fillings or composite veneers, to mask the discoloration.
Severe Cases
- Veneers.
- Crowns.
References
- Niazi FC, Pepper T. Dental Fluorosis. [Updated 2023 Jun 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK585039/
- C. M. Marya - A Textbook of Public Health Dentistry, Jaypee Brothers Medical Publishers (P) Ltd (2011). https://amzn.to/3SHP36G
- S. S. Hiremath - Textbook of Public Health Dentistry, Elsevier India (2016). https://amzn.to/49mh2jw
- The image used is licensed under the Creative Commons Attribution-Share Alike 4.0 International license. (Author: MoninaCisneros)
*This article is an excerpt from the above mentioned sources and Medical Sutras does not make any ownership and affiliation claims.