Adaptations are reversible changes in the number, size, phenotype, metabolic activity, or functions of cells in response to changes in their environment.
- Physiologic adaptations: Responses of cells to normal stimulation by hormones or endogenous chemical mediators e.g., hormone-induced enlargement of the breast and uterus during pregnancy, or to the demands of mechanical stress such as in case of bones and muscles.
- Pathologic adaptations: Responses to stress that allow cells to modulate their structure and function and thus escape injury, but at the expense of normal function, such as squamous metaplasia of bronchial epithelium in smokers.
The physiologic and pathologic adaptations can take several forms, that include,
- Hypertrophy.
- Hyperplasia.
- Atrophy.
- Metaplasia.
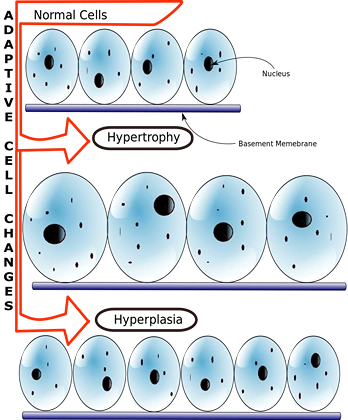
Hypertrophy
Refers to an increase in the size of cells resulting in an increase in the size of the organ. There are no new cells formed, just bigger cells containing increased amounts of structural proteins and organelles.
It occurs when cells have a limited capacity to divide and can be caused due to either increased functional demand or by growth factor or hormonal stimulation.
Physiologic Hypertrophy
- Enlargement of uterus during pregnancy: Due to estrogen-stimulated smooth muscle hypertrophy and hyperplasia.
- Hypertrophy of striated muscle cell in skeletal muscle & heart: In response to increased workload.
Pathologic Hypertrophy
- Cardiac enlargement associated with hypertension or aortic valve disease: Caused by mechanical triggers such as stretch, and soluble mediators such as growth factors and adrenergic hormones.
*Hypertrophy can progress to functionally significant cell injury, if the stress is not relieved, as there is a limit beyond which muscle enlargement can not compensate for the increased stress. For example, in the heart degenerative changes such as fragmentation and loss of myofibrillar contractile elements occurs, which ultimately leads to ventricular dilation and cardiac failure.
Hyperplasia
Refers to an increase in the number of cells in an organ that results from increased proliferation of differentiated cells or less differentiated progenitor cells.
It occurs in tissues that contain cells capable of replication, and may occur concurrently with hypertrophy.
Physiologic Hyperplasia
- Hormonal hyperplasia: Induced by hormonal changes, e.g., proliferation of glandular epithelium of the female breast at puberty and during pregnancy.
- Compensatory hyperplasia: Growth of residual tissue after removal or loss of part of an organ. e.g., when part of liver is resected, mitotic activity in the remaining cells restores the liver to normal size (stimulus: polypeptide growth factors produced by uninjured hepatocytes and nonparenchymal cells in the liver).
Pathologic Hyperplasia
- Endometrial hyperplasia & abnormal menstrual bleeding: Caused by increased estrogenic stimulation due to disturbance in the balance between stimulatory effects (of pituitary hormones and ovarian estrogen), and the inhibitory effects (of progesterone).
- Benign prostatic hyperplasia: Induced in response to hormonal stimulation by androgens.
- Hyperplasia associated with viral infection: e.g., papillomavirus cause skin warts and mucosal lesions that are composed of masses of hyperplastic epithelium.
*In all cases of hyperplasia, the growth of cells remains controlled and if the initiating signals are removed, hyperplasia disappears. This responsiveness to normal regulatory control mechanisms differentiates hyperplasia from cancer.
Atrophy
Refers to the shrinkage in the size of cells by the loss of cell substance. This leads to reduction in size (atrophy) of the entire tissue or organ when large number of cells are involved.
The atrophic cells are not dead and have diminished function. They represent a retreat to a smaller size at which survival is still possible, wherein a new equilibrium is achieved between cell size and diminished blood supply, nutrition or trophic stimulation.
Mechanisms
- Decreased protein synthesis, because of reduced metabolic activity.
- Increased protein degradation, mainly by the ubiquitin-proteasome pathway. (Nutrient deficiency and disuse may activate ubiquitin ligases.)
- Autophagy, wherein the starved cell eats its own organelles in an attempt to survive.
Etiology/Causes
- Decreased workload e.g., immobilisation of limb to allow healing after fracture.
- Loss of innervation.
- Diminished blood supply.
- Inadequate nutrition.
- Loss of endocrine stimulation.
- Aging (senile atrophy).
Metaplasia
Refers to the change in the phenotype of adult differentiated cells, i.e., one adult cell type (epithelial or mesenchymal) is replaced by another adult cell type.
In metaplasia, a cell type sensitive to a particular stress is replaced by another cell type better able to withstand the adverse environment. This is thought to arise by the reprogramming of stem cells to differentiate along a new pathway, rather than transdifferentiation of already differentiated cells (phenotypic change).
Examples:
- Respiratory epithelium of habitual cigarette smokers: Replacement of normal ciliated columnar epithelium by stratified squamous epithelium.
- Vitamin A deficiency: Vitamin A is essential for normal epithelial differentiation and its deficiency may induce squamous metaplasia in the respiratory epithelium.
- Chronic gastric reflux: The normal stratified squamous epithelium of the lower esophagus may change to gastric or intestinal-type columnar epithelium.
*If the triggers for metaplasia is persistent, they may predispose to malignant changes in the tissue.
References
- Robbins Basic Pathology, 10th edition, Vinay Kumar, Abul K. Abbas, Jon C. Aster, Elsevier.
- The image used is licensed under the Creative Commons Attribution-Share Alike 3.0 Unported license. (Author: SchwarzeMelancholie, Source: https://commons.wikimedia.org/wiki/File:Hyperplasia_vs_Hypertrophy.svg).
*This article is an excerpt from the above mentioned book and Medical Sutras does not make any ownership or affiliation claims.