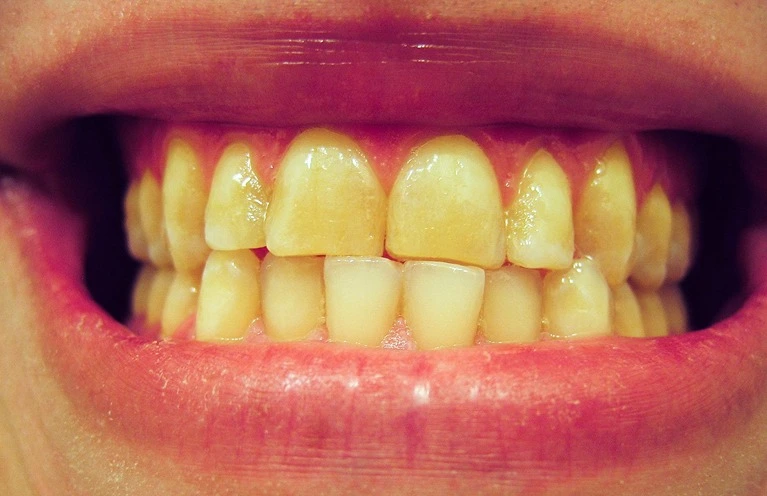
Bruxism can be defined as non-functional, habitual contact of teeth, that may include grinding or gnashing, clenching and tapping of the teeth.
Types
Daytime/Diurnal Bruxism
- Conscious or subconscious grinding of teeth usually during the day, usually silent except in patients with organic brain disease.
- It can occur along with parafunctional habits such as chewing pencils, nails, cheeks and lips.
Night time/Nocturnal Bruxism
- Subconscious grinding of teeth characterised by rhythmic patterns of masseter EMG activity.
Etiology
-
Occlusal discrepancies (Faulty restorations, deflective occlusal contacts, malocclusion): Can be attributed to the alteration of definite afferent impulses, originating in the periodontium.
-
Psychological factors (Nervous tension): Repressed anger, aggression, anxiety, etc.
-
CNS disturbances such as cortical lesions, cerebral palsy, mental retardation and tuberculous meningitis.
-
Hereditary factors such as children of bruxing parents.
-
Allergy: Nocturnal bruxism may be initiated reflexly by increased negative pressures in the tympanic cavities from intermittent allergic edema of the eustachian tube mucosa.
-
Other oral habits such as chronic biting and chewing of toys and pencils, thumb- and finger-sucking, tongue thrusting and mouth breathing.
-
Systemic factors:
- Magnesium deficiency.
- GI disturbances from food allergies, enzymatic imbalances, leading to chronic abdominal distress.
- Subclinical nutritional and vitamin deficiencies,
- Endocrine disorders eg. hyperthyroidism.
-
Occupational factors: Over enthusiastic students, compulsive over achievers or athletes.
Clinical Manifestations
The signs and symptoms of bruxism depends on the frequency, intensity and the age of the patient.
Dental Findings
- Increased tooth mobility (may be more in the morning).
- Non-functional patterns of occlusal wear and atypical wear facets.
- Increased tooth sensitivity (due to excessive abrasion of enamel).
- Dull percussion sounds.
- Soreness to biting stress.
- May cause fracture of restoration or root fracture.
- Sometimes, pulp may be exposed due to attrition, leading to dental abscess.
- Bruxism might be an essential factor for the spread of gingivitis into deeper periodontal structures and alveolar bone loss.
Musculature
- Tenderness of the jaw muscles, commonly lateral pterygoid and masseter muscles.
- Muscular fatigue or tightness on waking up.
- Hypertrophy of the masseter muscle (unilaterally/bilaterally).
- Order of muscle sensitivity: Lateral pterygoid -> Medial pterygoid -> Masseter.
TMJ Findings
- Pain in the joints, usually dull and unilateral.
- Crepitation and clenching within the joint.
- Restriction of mandibular movements.
- Deviation of chin during mandibular movements.
- The disc may become worn or perforated and wear patterns are often correlated with condylar remodelling.
Other Findings
- Chronic headaches and facial pain (often of muscular contraction type).
- Grinding and tapping sounds.
- Soft tissue trauma.
- Small ulcerations or ridging on the buccal mucosa opposite the molar teeth.
- There is a comorbidity between obstructive sleep apnea and nocturnal bruxism, and bruxism is included among the sleep-related movement disorders in the International Classification of Sleep Disorders.
Treatment
The various treatment modalities include:
- Occlusal adjustment (correction of any prematurities or occlusal interferences in restorations).
- Occlusal splint, Bite plane or Bite guard.
- Restorative treatment.
- Psychotherapy.
- Relaxation training.
- Medications.
- Electric method (electrogalvanic stimulation for muscle relaxation).
- Orthodontic treatment.
Occlusal Splint/Bite Plane/Bite Guard
- Vinyl bite guard that covers occlusal surfaces of all teeth can be worn at night to prevent continued abrasion.
- The occlusal surface of the bite guard should be flat to avoid occlusal interference.
- They also helps in passive stretching of painful muscle fibres by raising the bite.
Restorative Treatment
- Endodontic treatment with crown is indicated if the abrasion is severe and pulp exposure is imminent.
Psychotherapy
- Counselling the patient can lead to a decrease in tension and also create a habit awareness.
- Can lead to an increase in voluntary control and reduced tooth parafunction.
Relaxation Training
- In this technique, the patient is instructed to tense the muscle group in consideration and relax, thereby training the patient to relax the muscle group voluntarily.
- Hypnosis, conditioning, etc. are also indicated for subjects in whom bruxism is due to a central cause.
Medications
- Vapocoolants such as ethyl chloride for pain within the TMJ area.
- Local anaesthetic injections directly into the TMJ or into the muscles,
- Tranquilizers, sedatives and muscle relaxants.
- Placebos may be used to rule out psychological etiology.
- Medications such as diazepam may be prescribed for a few days to alter sleep arousal and anxiety level.
- Low doses of tricyclic antidepressants may be used to inhibit the amount of REM sleep.
Orthodontic Treatment
- Correction of malocclusion such as Class II and Class III, that may predispose to bruxism is recommended.
References
- McDonald and Avery's Dentistry for the Child and Adolescent (11th edition) -Mosby (2021).
- Textbook of Orthodontics (2nd Edition), Gurkeerat Singh, Jaypee Brothers Medical Publishers (P) Ltd.
- The image used is in public domain (Source : Wikimedia Commons).
*This article is an excerpt from the above mentioned books and Medical Sutras does not make any ownership or affiliation claims.