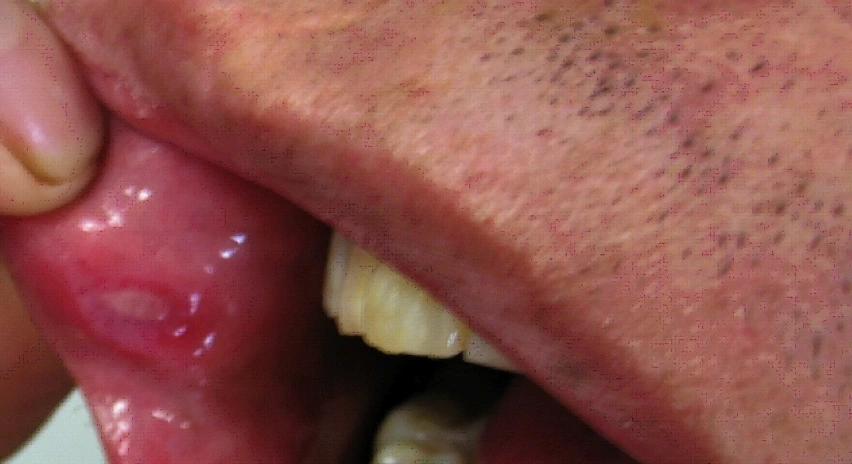
Was first described by Turkish dermatologist Hulusi Bechet as a triad of symptoms, consisting of recurring oral ulcers, recurring genital ulcers and eye involvement.
Etiology
- Abnormal immune response in a genetically susceptible host, characterised by systemic perivascularitis and hyperactivity of neutrophils with enhanced chemotaxis and elevated proinflammatory cytokines (IL-8, IL-17, and TNF-A).
- Most frequently linked with HLA-B51 genotype (60% of patients).
- Environmental factors : Organophosphates, Organochlorides, Heavy metal intoxication, and allergens.
- Oral microbiota : Streptococcus sanguis and Streptococcus oralis.
Clinical Findings
-
Characterised by exacerbations and remissions, with duration of attacks ranging between few days to few weeks.
-
Oral mucosa is the most common site, followed by the genital area.
-
Oral manifestations :
- Recurring oral ulcers (90% of patients) : usually the first to appear, and similar clinically and histologically to Reccurent Aphthous Stomatitis.
-
Genital lesions :
- Males : Ulcers of the scrotum and penis.
- Females : Ulcers of the labia.
-
Ocular lesions :
- Photophobia and irritation.
- Conjunctivitis, Uveitis, Retinal vasculitis.
- Hypopyon.
- Vascular occlusion.
- Optic atrophy.
-
Skin lesions (50% of patients) :
- Papulopustular lesions (acneiform) or pseudofolliculitis.
- Erythema nodosum.
- Superficial thrombophlebitis.
- Cutaneous ulcers and nodules.
- Cellulitis type lesions.
-
Complications :
- Blindness.
- Thrombosis and embolism.
- Rupture of large-vessel aneurysms.
- Arthritis (40% of cases).
- CNS Involvement - Brainstem syndrome, involvement of cranial nerves, or nerve degeneration resembling multiple sclerosis.
- Thrombophlebitis.
- Intestinal ulceration.
- Renal, Cardiac and Pulmonary involvement.
International Criteria for Bechet's Disease 2010
- A score of 4 or more points predicts Bechet's disease with 95% certainity, 98% if the pathergy test is performed.
- Oral Aphthous Stomatitis (3 or more attacks in one year) : 2 points.
- Genital Ulceration (Recurrent ulcers or scarring) : 2 points.
- Ocular Lesions (Uveitis or retinal vasculitis) : 2 points.
- Skin Lesions (Follicular pustular rash or erythema nodosum) : 1 point.
- CNS involvement (Any involvement) : 1 point.
- Vascular Manifestations (Superficial phlebitis, deep vein thrombosis, large vein thrombosis, arterial thrombosis, and aneurysm) : 1 point.
- Positive Pathergy Test (optional) : 1 point.
Laboratory Findings
- Hypergammaglobulinemia.
- Leukocytosis with eosinophilia.
- Elevated ESR, C-reactive protein and C3, C4 complements, during the active phases of disease.
- Platelet rosette formation around neutrophils, seen in acute phases (disappear after recovery).
Management
- Depends on the severity and sites of involvement.
- Requires multidisciplinary approach, with the goal to prevent irreversible organ damage.
- Cyclosporine and Tacrolimus are the main treatments, with steroids for acute exacerbations.
- Thalidomide and topical tacrolimus are most effective for oral ulcers.
- Systemic therapy with colchicine, pentoxifylline, and dapsone is often useful when mucocutaneous lesions are frequent or severe.
- In refractory cases, thalidomide, azathioprine, or biological agents such as TNF-A antagonists (Infliximab, Etanercept) and interferon-alpha, may be necessary.
Points to Note
- Hypopyon is a visible layer of pus (exudate rich in white blood cells) seen in the anterior chamber of eye (found in 12% of cases).
- Blindness is a possible complication of Bechet's disease and hence, periodic evaluation by an ophthalmologist is necessary.
- Pathergy test (Neutrophilic vascular reaction of leukocytoclastic vasculitis) : The doctor inserts a 20-gauge or smaller needle obliquely into the skin under sterile conditions and checks for 24-48 hours, how the immune system reacts to a minor injury.
References
-
Burket's Oral Medicine, 13th Edition, Michael Glick, Martin S. Greenberg, ,Peter B. Lockhart, Stephen J. Challacombe, Wiley Blackwell.
-
Shafer, Hine, Levy Shafer's Textbook of Oral Pathology (7th Edition), Editors - R Rajendran, B Sivapathasundharam, Elsevier.
-
Cawson's Essentials of Oral Pathology and Oral Medicine, 9th Edition, EW Odell, Elsevier.
-
Contemporary Oral Medicine, A Comprehensive Approach to Clinical Practice, Camile S Farah, Ramesh Balasubramaniam, Michael J Mccullough, Springer.
-
Anil Govindrao Ghom, Savita Anil Ghom (Lodam) - Textbook of Oral Medicine - Jaypee Brothers Medical Publishers (P) Ltd (2014).
-
The image used is licensed under the Creative Commons Attribution-Share Alike 3.0 Unported license.
- Description : Bechets disease Oral Ulcer in patient with the disease.
- Source : http://dermatology.cdlib.org/1611/articles/18_2009-10-20/2.jpg.
- Author : Ahmet Altiner MD, Rajni Mandal MD.
*This article is an excerpt from the above mentioned books and Medical Sutras does not make any ownership or affiliation claims.