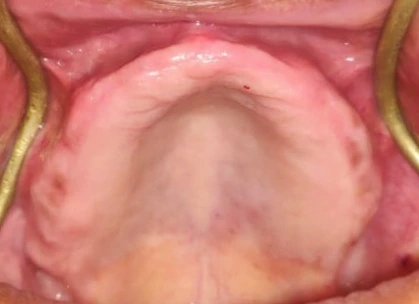
The average denture bearing area available for support in edentulous maxilla : 24 cm2.
The bone and covering soft tissues forms the foundation for dentures. Short-term and long term health of the contacting tissues is influenced by the methods used to capture these tissues and the final adaptation of the denture bases in function.
Mucous Membrane
It is composed of mucosa and submucosa.
Mucosa
-
Mucosa is formed by stratified squamous epithelium and lamina propria (narrow layer of connective tissue).
-
Masticatory mucosa
- Characterised by well defined keratinised epithelium and lack of tissue movement.
- Covers the hard palate and crest of the residual ridge, in edentulous patients, and residual attached gingiva.
-
Lining mucosa
- Devoid of the keratinised layer.
- Freely movable with the tissues to which it is attached because of the elastic nature of the lamina propria.
- Found in the vestibular spaces, lips and cheeks, alveololingual sulcus, soft palate, ventral surface of the tongue and unattached gingiva of the slopes of residual ridge.
Submucosa
- Formed by connective tissue that varies in thickness and may be characterised by dense or loose areolar tissue.
- Transmits the blood and nerve supply to the mucosa and may also contain glands, fat or muscle fibres.
- The thickness and consistency of submucosa are largely responsible for providing support to a denture, as it makes the bulk of the mucous membrane, .
- When the submucosa is thin : Soft tissue will be resilient and mucous membrane will be easily traumatised.
- When submucosa is loosely attached to the periosteum, inflamed or edematous : Adversely affects the stability and support, as the tissue becomes easily displaceable,
Stress Bearing or Supporting Areas
The primary stress bearing areas generally have thicker mucosa and/or underlying cortical bone that is less subject to resorption. These include :
- Maxillary tuberosities.
- Hard palate on either side of palatal raphe.
The secondary stress bearing areas are made up of cancellous bone and subject to resorptive remodelling after dental extraction and with long-term denture wear. These include :
- Residual ridge.
- Palatine rugae.
Maxillary Tuberosities
- Consists of dense fibrous connective tissues with minimal compressibility, hence, provide considerable support to the denture.
- The need for surgical tuberosity reduction should always be evaluated, when the maxillary teeth are extracted : If maxillary teeth remain unopposed, the tuberosities and posterior alveolar arch can hyper-erupt below the occlusal plane, interfering with placement of the mandibular prosthetic dentition.
Hard palate
- The palatine process of maxilla (anteriorly) and the horizontal process of palatine bones (posteriorly) provide considerable surface area to provide support to the denture.
- The horizontal portion of the hard palate lateral to the midline forms the primary stress bearing area, as it is resistant to resorption.
- Anterolaterally, the submucosa contains adipose tissue, while, posterolaterally, it contains glandular tissue. Although, it contributes to support the denture, this tissue is displaceable,.
- Palatine rugae : Considered as secondary stress bearing area, since, it is covered by soft tissue and the palate is set at an angle to the residual ridge in the rugae area.
Residual ridge
-
It is considered a secondary stress bearing area, as it is made up of cancellous bone and is subject to resorptive remodelling after dental extraction and with long-term denture wear.
-
The submucosa is devoid of fat or glandular cells and characterised by dense collagen fibres that are contiguous with lamina propria.
-
Crest of the residual ridge :
- Mucosa is derived from the remnant gingival tissues and are excellent stress-bearing tissues.
- Also, the mucosa is firmly attached to the periosteum of the underlying bone by the connective tissue of the submucosa, hence provide adequate resiliency to support the denture.
- If a patient is edentulous for many years, the crest of residual ridge may lack a smooth, cortical bone under the mucosa.
-
Slope of the residual ridge :
- Mucous membrane loses its firm attachment to the underlying bone, has non-keratinised or slightly keratinised epithelium.
- Submucosa contains loose connective tissue and elastic fibres, will not withstand the forces of mastication.
- They provide stability against lateral displacement and create the peripheral seal.
Relief Areas
The areas requiring relief in impression includes :
- Secondary stress bearing areas.
- Palatal torus.
- Median palatal raphe.
- Incisive foramen.
- Undercuts or sharp bony prominence on ridges.
Torus palatinus
- Hard bony enlargement that occurs in the midline of the palate (20% of the population).
- It is covered by a thin layer of mucous membrane that is easily traumatised by the denture base, if relief is not provided.
- Even with slight amount of resorption of the residual ridge, the denture will rest heavily on the torus, resulting in disruption of previous retention : The retention can be improved by identifying the torus with pressure paste and minor adjustment.
- If the torus extends posteriorly to the vibrating line : It may need to be surgically reduced in order to achieve posterior palatal seal and adequate retention.
Median palatal raphe
-
Need to be relieved, since,
- Submucosa is extremely thin and the mucosal layer is practically in contact with the underlying bone.
- Soft tissue covering the medial palatal suture is non-resilient.
Incisive foramen
- Located beneath the incisive papilla, on a line immediately behind and between the central incisors
- The location of incisive papilla gives indication of the amount of resorption, since, it moves nearer to the crest of the ridge as resorption progresses.
- The nasopalatine nerves and blood vessels pass through the foramen, hence, the denture base should not impinge on them.
Root of the zygoma
- Lies distal to the buccal frenum, opposite the first molar region.
- Denture may require relief over this area to prevent soreness of the underlying tissue, since, with increasing resorption of the ridge, it becomes more noticeable.
Peripheral or limiting areas
The limiting structures of the upper arch can be divided as under,
- Labial border : Labial vestibule.
- Buccal border : Buccal vestibule.
- Distal limit : Hamular notch.
- Posterior border : Vibrating line.
Labial vestibule
-
It runs from one buccal frenum to the other on the labial side of the ridge.
-
Lined by non-keratinised lining mucosa with loose submucosa and an elastic lamina propria.
-
Can be divided into right and left labial vestibule by the labial frenum.
-
The outer surface of the labial vestibule is formed by orbicularis oris (main muscle of the lip, fibres pass horizontally from the lips and anastomoses with the fibres of buccinator, tone depends on the support it recieves from the labial flange and position of the teeth.
-
Labial frenum :
- Fold of mucous membrane at the midline, dividing the labial vestibule.
- It contains no muscle and has no action of its own.
- It starts superiorly in a fan shape and converges as it descends to attach on the labial side of the ridge.
- The labial notch in the denture must be just wide and deep enough to allow the frenum to pass through it as the patient moves the upper lip.
-
Buccal frenum :
- Forms the dividing line between the labial and buccal vestibules.
- The frena may be a single or double fold of mucous membrane or even a broad-fan shape.
- The buccal notch in the denture requires more clearance than labial notch, since the position of buccal frenum is affected by several muscles, i.e, levator anguli oris (attaches beneath the frenum), orbicularis oris (pulls the frenum forward) and buccinator (pulls it backward).
Buccal vestibule
-
It lies opposite the tuberosity and extends from the buccal frenum to the hamular notch.
-
Size of the buccal vestibule varies with,
- Contraction of buccinator muscle.
- Amount of bone lost from the maxilla.
- Position of the mandible : When the mandible opens or moves to the opposite side, the width of the buccal vestibule is reduced.
Hamular notch
- It is situated between the tuberosity and the hamulus of the medial pterygoid plate, and forms the distal limit of the buccal vestibule.
- Consists of thick submucosa made up of loose connective tissue.
- Distal end of the denture must cover the tuberosities and extend into the hamular notch : Overextension will not be tolerated because of pressure on the pterygoid hamulus and interference with the pterygomandibular raphe (extends from the hamular notch to the retromolar pad).
- When the mouth is opened wide, the pterygomandibular raphe is pulled forward -> If the denture extends too far into the hamular notch, the mucous membrane covering the raphe will be traumatised.
Vibrating line
- It is an imaginary line (always on the soft palate) drawn across the palate extending from one hamular notch to the other.
- It marks the beginning of the motion in the soft palate when an individual says "ah" and the soft palate elevates.
- It usually passes 1-2 mm in front of the fovea palatinae, at the midline.
- The distal end of the denture should extend to the vibrating line.
Points to Note
- The resorption of residual ridge is greatest in the first 6-12 months after extraction, but it continues at a reduced rate throughout life.
- Why to remove the dentures from the mouth at night, for 6-8 hours ? : This allows keratinisation to increase and dramatically reduces the signs of inflammation seen in the submucosa.
- It is critical to maintain all of the available attached gingival tissue when closing the extraction sites : The width of the residual ridge crest varies with the height of the attached gingiva at the time of extraction.
- Importance of well-fitting denture : Cytologic studies indicate that increased amounts of keratinised material are present in edentulous ridges when the clinical quality of the dentures is good.
- Stimulation of the mucosa of the residual ridge through toothbrush physiotherapy also increases the presence of keratinised material.
- The extent of buccal vestibule should be examined with the mouth as nearly closed as possible : When the mouth is opened wide, the coronoid process obscure the buccal vestibule.
- Fovea palatinae : Indentations near the midline of the palate formed by a coalescence of several mucous gland ducts. They are always in soft tissue, which makes them an ideal guide for the location of posterior border of the denture.
References
- Prosthodontic Treatment for Edentulous Patients Complete Dentures and Implant-supported Prostheses (13th edition) , Zarb, Hobkirk, Eckert, Jacob, Mosby Elsevier.
*This article is an excerpt from the above mentioned book and Medical Sutras does not make any ownership and affiliation claims.