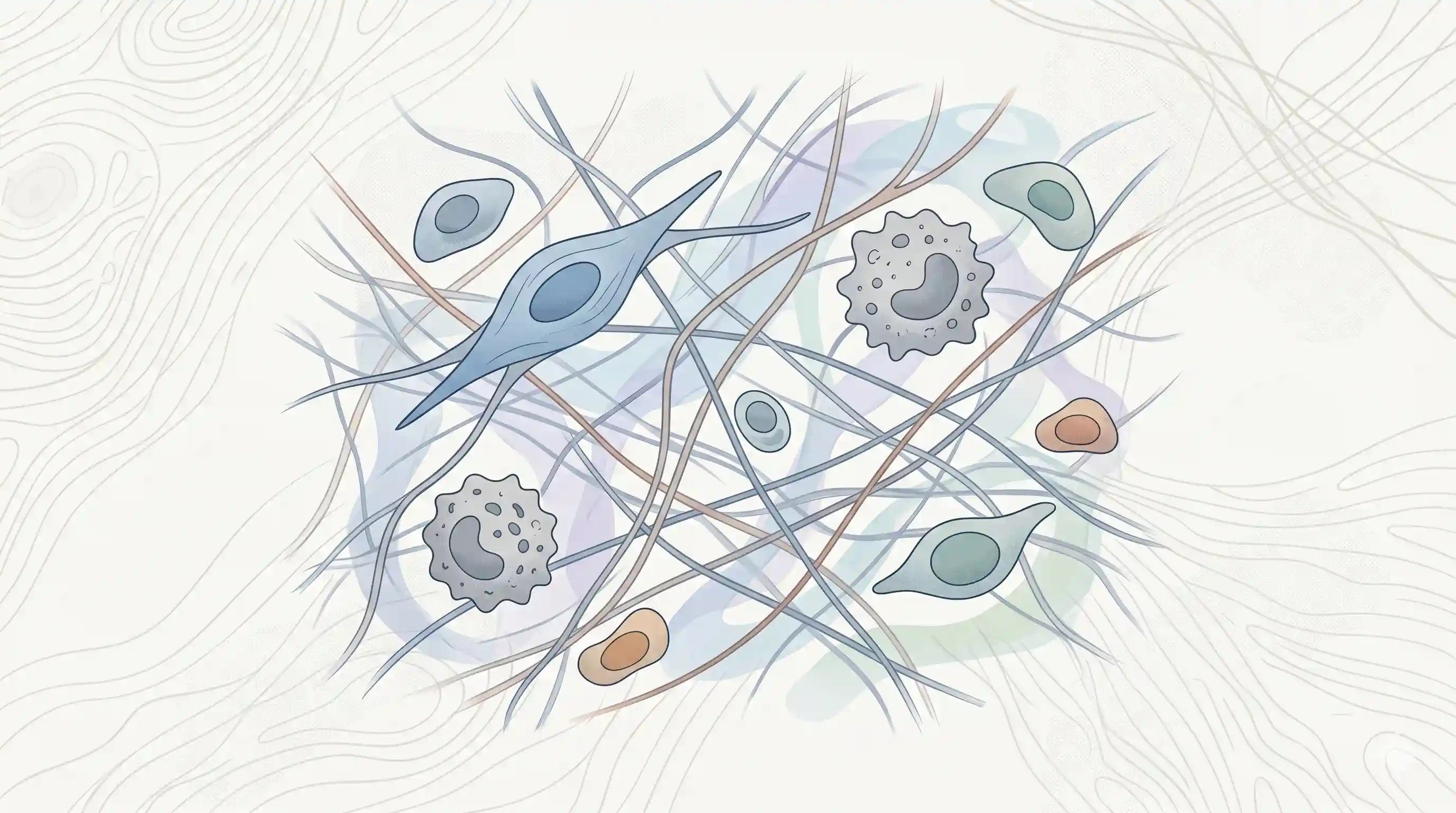
Connective tissue functions as the vital biological scaffolding of the human body, constructed from a dynamic interaction between resident cells and the extracellular matrix (ECM) they synthesize and maintain. The ECM consists of structural protein fibers (collagen, elastin, and reticular fibers) embedded in a highly hydrated, gel-like ground substance that collectively dictate the tissue's biomechanical and metabolic properties.
Resident & Transient Cells
- Fibroblasts: The predominant, architecturally crucial cells of connective tissues. They are uniquely capable of simultaneously synthesizing and degrading ECM components. Active fibroblasts feature a large, vesicular (open-faced) euchromatic nucleus, an extensive rough endoplasmic reticulum (RER), and a prominent Golgi complex.
- Macrophages (Histiocytes): Derived from circulating monocytes, these irregularly shaped cells contain abundant lysosomes and phagosomes. They orchestrate tissue repair by phagocytosing debris and releasing critical growth factors (TGF-β, PDGF) and cytokines that stimulate fibroblast proliferation and angiogenesis.
- Mast Cells: Large, round cells frequently situated adjacent to blood vessels. Their cytoplasm is packed with deeply basophilic, metachromatic granules containing histamine and heparin. They play critical roles in initiating the vascular phase of inflammation and regulating endothelial proliferation.
- Undifferentiated Mesenchymal Cells: Pluripotent, spindle-shaped stem cells generally occupying a perivascular location. They serve as a critical cellular reservoir, capable of differentiating into odontoblasts, fibroblasts, or macrophages in response to injury or physiologic demand.
- Plasma Cells: Transient defense cells seen during pulpal or mucosal inflammation. They feature a distinct "clock face" or "cartwheel" nucleus with peripherally clumped chromatin and intensely basophilic cytoplasm. Their primary function is the synthesis of antibodies (immunoglobulins).
Extracellular Matrix (Fibers)
- Type I collagen: It is the most abundant structural protein, constituting the vast majority of the organic matrix in bone, dentin, cementum, and the PDL, and providing immense tensile strength.
- Type III collagen: Found in fine, argyrophilic (silver-staining) reticular fibers. It is highly prevalent in the dental pulp, embryonic connective tissues, and at the periphery of Sharpey's fibers.
- High-Yield Synthesis Pathway: Synthesis begins in the RER with the translation of pro-alpha chains. Prolylhydroxylase and lysylhydroxylase (enzymes strictly dependent on Vitamin C) hydroxylate proline and lysine residues, permitting interchain hydrogen bonding. Three chains weave into a triple helix (procollagen). Following exocytosis, extracellular procollagen peptidases cleave terminal extensions, allowing molecules to self-assemble into staggered fibrils. Finally, the extracellular enzyme lysyl oxidase forms covalent intermolecular cross-links to mature and stabilize the fibril.
- Elastic Fibers:
- Mature Elastin: Consists of an amorphous elastin core surrounded by microfibrils.
- Elaunin Fibers: Immature elastic fibers consisting of bundles of microfibrils embedded in a small amount of amorphous elastin (found in the gingival ligament).
- Oxytalan Fibers: Immature elastic fibers consisting only of a microfibrillar component (composed of fibrillin and type IV collagen). In the PDL, they run perpendicular to the occlusal plane to support and protect the walls of blood vessels.
Ground Substance
A highly hydrated, amorphous matrix through which all metabolic exchange occurs. It consists of glycosaminoglycans (e.g., hyaluronan), proteoglycans (e.g., decorin, versican, syndecan), and adhesive glycoproteins (e.g., fibronectin, tenascin). Fibronectin bridges the cellular cytoskeleton to the ECM via transmembrane integrin receptors.
- Hydration and Function: The ground substance is highly hydrated (e.g., 70% water in the PDL), which acts as a hydraulic cushion to dissipate heavy masticatory stress loads and serves as the medium for the diffusion of metabolic nutrients and waste.
- Glycosaminoglycans (GAGs): Long, unbranched chains of repeating disaccharide units. Because they are highly acidic and negatively charged, they are intensely hydrophilic. Hyaluronan (hyaluronic acid) is the major GAG in early development and forms viscous hydrated gels. Dermatan sulfate is the principal GAG in the mature PDL.
- Proteoglycans: Formed when GAGs covalently bond to a protein core. Important examples include decorin (assists in collagen fibrillogenesis), versican, biglycan, and syndecan (a transmembrane proteoglycan involved in cell-matrix adhesion).
- Glycoproteins: Adhesive molecules containing a polypeptide chain with simple hexoses. Fibronectin is the predominant adhesive glycoprotein; it bridges the cellular cytoskeleton (via transmembrane integrin receptors) to extracellular collagen fibrils, facilitating cell attachment and migration.
🩺 Dental/Clinical Significance
- Periodontal Ligament (PDL) Remodeling: The PDL is a highly specialized connective tissue exhibiting one of the fastest collagen turnover rates in the human body. PDL fibroblasts perform dual roles: synthesizing new Type I and Type III collagen while simultaneously degrading older fibrils via intracellular phagolysosomes. This rapid, continuous remodeling is the biologic foundation that permits orthodontic tooth movement and adaptation to heavy masticatory forces without scar formation.
- Dental Pulp Dynamics: The pulp is a loose connective tissue entirely encased within rigid dentinal walls. It contains a high proportion of Type I and Type III collagen, abundant ground substance (which creates high tissue-fluid pressure), but completely lacks mature elastic fibers. During severe inflammation (pulpitis), the inability of the rigid chamber to expand can lead to vascular compression, ischemia, and subsequent pulpal necrosis. Conversely, surviving pulpal fibroblasts and undifferentiated mesenchymal cells can secrete angiogenic factors and differentiate into odontoblast-like cells to form tertiary (reparative) dentin in response to caries or cavity preparation.
- Vitamin C Deficiency (Scurvy): Because the hydroxylation of procollagen in the RER is Vitamin C-dependent, a deficiency prevents the formation of stable collagen triple helices. Tissues with high turnover rates like the periodontal ligament are affected first, clinically manifesting as the loosening and eventual loss of teeth.
📝 High Yield Exam Points
- Collagen Assembly & Banding: Procollagen is synthesized in the RER and processed in the Golgi. Once secreted, molecules self-assemble extracellularly in a staggered array, creating a characteristic 64 nm (640 Å) transverse banding pattern.
- Vitamin C Dependency: The enzymes prolylhydroxylase and lysylhydroxylase, which hydroxylate proline and lysine residues in the RER to allow stable triple-helix formation, are strictly dependent on Vitamin C
References
- Nanci, A. Ten Cate’s Oral Histology: Development, Structure, and Function. Elsevier (2018).
- Kumar, G. S. Orban's Oral Histology & Embryology. Elsevier (2019).
*This article is excerpt from the above mentioned sources and Medical Sutras does not make any ownership and affiliation claims.